The best Neurological Emergencies treatment: Understanding and Managing Critical Conditions
Introduction: Neurological emergencies are critical conditions that require immediate medical attention due to their potential to cause severe damage to the nervous system. Among the most common neurological emergencies are stroke, traumatic brain injury (TBI), and spinal cord injury (SCI). In this blog, we will delve into these neurological emergencies, exploring their causes, symptoms, and the urgent treatment approaches employed to minimize long-term complications and optimize patient outcomes.
- Stroke: A Medical Emergency: Stroke is a neurological emergency characterized by a sudden disruption of blood supply to the brain, leading to brain cell damage. Ischemic stroke, caused by a blood clot, and hemorrhagic stroke, resulting from bleeding in the brain, are the two primary types. Common symptoms include sudden weakness or numbness, difficulty speaking or understanding speech, severe headache, and loss of balance or coordination. When a stroke is suspected, immediate medical intervention is crucial. Treatment options may include thrombolytic therapy, mechanical clot retrieval, and supportive care to manage symptoms and prevent further brain damage.
- Traumatic Brain Injury (TBI): Impact and Consequences: Traumatic brain injury occurs as a result of a sudden blow or jolt to the head, leading to damage to the brain tissue. It can range from mild concussions to severe injuries. Symptoms may include confusion, loss of consciousness, memory loss, headaches, dizziness, and changes in mood or behavior. In a TBI emergency, prompt medical evaluation is essential to assess the severity of the injury. Treatment may involve stabilization of vital signs, neuroimaging scans to assess brain damage, surgical interventions to relieve pressure or remove hematomas, and a comprehensive care plan to address physical, cognitive, and emotional challenges during the recovery process.
- Spinal Cord Injury (SCI): Protecting the Central Nervous System: Spinal cord injuries result from trauma that damages the spinal cord, leading to temporary or permanent changes in sensation, movement, and bodily functions. Common causes include falls, motor vehicle accidents, and sports-related incidents. Symptoms depend on the level and severity of the injury and may range from localized pain to complete paralysis. In a spinal cord injury emergency, immobilization of the spine is crucial to prevent further damage. Treatment may involve surgery to stabilize the spine, medication to reduce swelling, rehabilitation to regain function, and ongoing management of secondary complications such as respiratory issues, muscle spasticity, and bladder or bowel dysfunction.
- Immediate Steps and Medical Intervention: When facing a neurological emergency, time is of the essence. Recognizing the symptoms and promptly seeking medical attention can significantly impact patient outcomes. Emergency medical services should be contacted immediately, and patients should be transported to the nearest stroke or trauma center equipped to handle neurological emergencies. Upon arrival, a multidisciplinary medical team will conduct a thorough evaluation, which may include imaging scans, laboratory tests, and neurological assessments. Treatment plans will be tailored to the specific condition, with a focus on stabilizing vital signs, ensuring adequate oxygenation and blood flow, managing pain and swelling, and preventing further injury or complications.
Conclusion: Neurological emergencies, such as stroke, traumatic brain injury, and spinal cord injury, demand urgent medical attention to minimize long-term damage and optimize patient outcomes. Recognizing the symptoms and seeking immediate medical help is vital in these critical situations. Healthcare professionals with expertise in neurology and emergency medicine are equipped to diagnose and manage these emergencies using a multidisciplinary approach. Timely interventions, including medical therapies, surgical procedures, and rehabilitation, are implemented to address the specific needs of each patient. By raising awareness about neurological emergencies, their causes, symptoms, and treatment approaches, we can ensure that individuals understand the importance of seeking prompt medical care and taking preventive measures when possible. Additionally, it is crucial to emphasize the significance of adopting safety precautions to reduce the risk of neurological emergencies, such as wearing protective gear during sports activities, following traffic safety regulations, and maintaining a healthy lifestyle to minimize the chances of stroke.
In summary, neurological emergencies pose a significant threat to the nervous system and require immediate medical attention. Understanding the symptoms and risk factors associated with conditions like stroke, traumatic brain injury, and spinal cord injury can empower individuals to take appropriate action and seek timely help. By raising awareness, promoting safety measures, and ensuring access to specialized medical care, we can collectively work towards reducing the impact of neurological emergencies, improving patient outcomes, and enhancing overall neurological health.
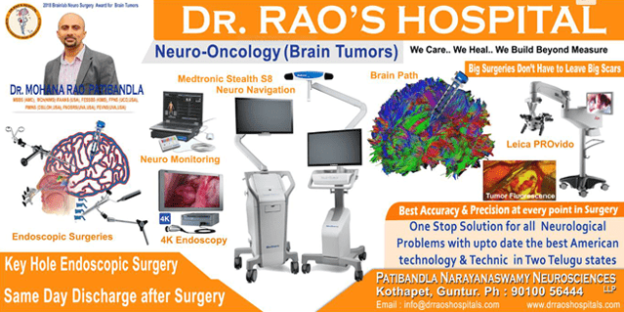
When it comes to addressing neurological emergencies, individuals can find solace in the expertise and exceptional care provided at Dr. Rao’s Hospital in Guntur. Led by the esteemed Dr. Rao, renowned as the best neurosurgeon in India, the hospital stands as a beacon of excellence in neurocritical care and emergency neurosurgery. With a dedicated team of skilled healthcare professionals, state-of-the-art facilities, and advanced medical technologies, Dr. Rao’s Hospital is at the forefront of managing critical neurological conditions with precision and compassion. Patients can trust in the hospital’s unwavering commitment to delivering optimal outcomes, providing comprehensive and personalized treatment plans, and ensuring that every aspect of their care is prioritized. Whether it is stroke management, traumatic brain injury interventions, or prompt response to spinal cord emergencies, Dr. Rao’s Hospital combines expertise, experience, and a patient-centric approach to create a truly exceptional neurosurgical care environment.
#NeurologicalEmergencies #StrokeEmergency #TraumaticBrainInjury #SpinalCordInjury #EmergencyCare #Neurology #CriticalConditions #UrgentMedicalAttention #BrainHealth #NeurologicalRecovery