Medical Myths: Everything You Need to Know About Epilepsy
Epilepsy is a brain disorder that causes recurrent seizures. It is often difficult for people living with epilepsy to understand what it means to have a seizure and the life-altering consequences of the condition.
Learning about medical myths can help patients decrease the confusion, uncertainty, and fear they may feel about their diagnosis.
Myths about epilepsy can lead to misunderstanding and misinformation. There is no one medical myth that revolves around epilepsy; rather, they are common misconceptions that can be found in different communities and organizations.
The myths surrounding epilepsy can lead to unnecessary fear and anxiety.
Medical myths are false beliefs about medicine that people believe despite the evidence against them. They can range from incorrect information about how a drug works, the proper dosage of a medication, or common side effects associated with a medication.
People will often continue to believe in these types of myths because they feel that their doctor has made a mistake when recommending these medications or treatments.
Dr Rao’s hospital in Guntur, Andhra Pradesh is the best center for the epilepsy surgery and epilepsy treatment. It also has epileptologist and neurosurgeon Dr. Mohana Rao Patibandla, who trained in epilepsy surgery in the united states that participates in identification of the source of the epilepsy, its treatment and its management.
Myths About Epilepsy
Dr. Mohana Rao Patibandla, USA fellowship trained epilepsy surgeon explains the myths of epilepsy and need for the correct understanding about the epilepsy.Epilepsy affects anyone who has seizures:
All the Epilepsy is not a genetic condition with which people are born with it. The disease is caused by damage to the brain, and people who have seizures do not have an underlying brain problem.
Epilepsy is not contagious. It also does not mean that the person is likely to have another seizure in the future; they are only at higher risk of having another seizure, because they already have had one, or because their seizures are severe and difficult to control, requiring more treatment options.
All the patients of epilepsy have shaking body movements:
Epilepsy can affect more than one part of the body at the same time. But there are several different seizure patterns that epileptic individuals can experience. Some of them have the staring look, some of them stutter, some have flashing of light, some have laughter, some will have fear etc these are some examples of the seizures.
Although treatment varies from person to person, there is no single treatment for every type of epilepsy; rather, a combination of medications and lifestyle changes may be needed to achieve good seizure control for each patient.
Epileptics are unable to work:
People with uncontrolled seizures may be able to use medical leave and accommodations, such as flexible working schedules, that can help them continue to work.
Epileptics are dangerous:
Epilepsy is not a mental illness, and it does not cause someone to become violent or unpredictable. People with epilepsy are not likely to hurt themselves or others around them.
People with uncontrolled seizures may need additional medical care or supervision when they are having a seizure; however, in general, epileptics are able-bodied and safe to work alongside their coworkers.
Epilepsy is a contagious disease:
It is unlikely to become contagious from a healthy person to someone with epilepsy. It is possible to get a fever or infection from a person with epilepsy who has had an intense seizure and does not drink enough fluids.
However, it is unlikely for someone with epilepsy to pass this on to others through casual conversation.
Epilepsy can be caused by a variety of factors, including the following:
– After a head injury (See Traumatic brain injury)
– After a stroke
– Genetics
– Various infections, including meningitis, encephalitis, and abscesses in the brain
– Brain infections, including HIV
– Low oxygen levels before birth
– Worms or parasites inside or near the brain or spinal cord
– Complications from a difficult birth (See Prenatal conditions)
Epilepsy patients are emotionally unstable:
It is common for many people with epilepsy to have some degree of emotional instability. But this group of patients is not likely to be emotionally unstable. It is important to remember that while everyone experiences mood changes.
Depression and anxiety, which can cause emotional instability, these symptoms are usually not caused by epilepsy. Epilepsy patients are generally able to handle uncomfortable emotions healthily because they have been educated about the disease.
Epilepsy causes depression:
People with epilepsy are not more prone to developing depression than people who do not have the condition.
In addition, studies have shown that people with epilepsy may be less prone to depression or anxiety than non-epileptic individuals.
Epilepsy is a psychological condition:
Epilepsy is a neurological condition that is not caused by psychological disorders. However, epileptics often experience a great deal of fear and anxiety due to their condition.
They may develop depression or anxiety in response to the stress of living with a chronic illness. Epilepsy has also been linked to affective disorders such as schizophrenia and bipolar disorder. But these conditions are not caused by epilepsy itself.
During seizures, all the persons with epilepsy lose consciousness and convulse:
Not all people with epilepsy have seizures that cause loss of consciousness or loss of muscle control.
A seizure can have different characteristics, and people with epilepsy may experience seizures that cause loss of consciousness or convulsions.
Moreover, some people with epilepsy have seizures without warning, even during sleep (called “sleep seizures”) or withdrawal from medication “withdrawal seizures”.
Epileptics should not become pregnant:
People with epilepsy can safely become pregnant, and being pregnant does not worsen their condition. Getting pregnant and becoming a parent may help patients control their seizures by giving them something else to focus on.
However, if they have complex or refractory epilepsy, they may be advised to wait until the condition is well controlled.
It is dangerous for someone suffering from epilepsy to go out in public:
Seizures can have different types, and they can occur at any time of the day or night.
This myth may arise because some seizures are more likely to occur during particular times of the day with certain triggers such as stress, lack of sleep and fatigue.
During a seizure, people frequently swallow their tongue:
Most people with epilepsy do not swallow their tongue during a seizure. If they are near water, however, they may aspirate water into their lungs and experience drowning.
The likelihood of this happening is even lower in an epileptic individual with a functioning airway (for example, in someone who has recently had an episode).
In epileptic patients, strobe lights always cause seizures:
This myth is based upon a series of cases where epileptic patients were exposed to strobe lights. Seizures were observed in those patients, and no actual seizures were observed by those researchers who conducted the testing.
This is false, however, an epileptic patient should be extra careful when in the light of a strobe light.
Epileptics are impulsive, angry and prone to antisocial behaviour:
Many people with epilepsy are very calm and friendly.
This myth may arise because epileptic individuals often have difficulty controlling their impulses or behaviour because of the seizures and their medications.
If someone is suffering from a seizure, it is best to restrain them:
Restraint should always be done with care and great caution. Aside from the fact that restraint may cause injury to the patient.
It does not stop a seizure from the beginning or keeps it from spreading. The only way to prevent a seizure is with medication or surgery.
There are no effective therapies for epilepsy to cure or to control the seizures.
Several types of epilepsy syndromes have been identified:
The treatment of epilepsy varies according to the type of seizure, severity, whether it is part of a syndrome and overall condition of the patient. Some general principles for treatment are as follows.
66% of epilepsy patients seizures are controlled by the medication itself and this is medically treatable epilepsy.
33% of seizures patients are not controllable with medciation and need to identify the focus of seizures so that they can be cured or controlled, these are called drug resistant epilepsy.
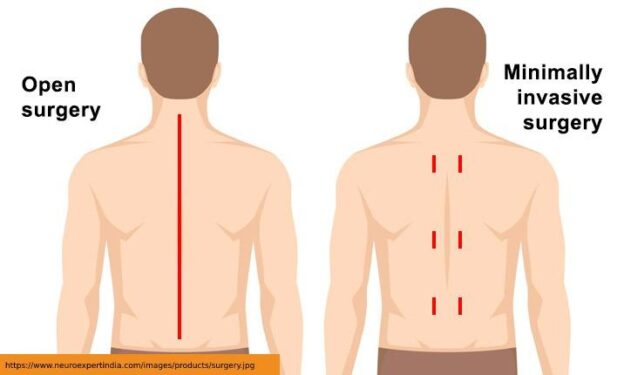
Many people with epilepsy can control their seizures with medications. However, others are not so fortunate. If a person with epilepsy is still having seizures after trying two medications over a period of 2 years are called drug resistant epilepsy and these are candidates for evaluation for surgery..
They may be a candidate for surgery to remove part of the brain that causes seizures in their area of the brain (lesion surgery). Sometimes metal electrodes are placed directly on the surface of the brain and connected directly to an implanted pulse generator. The pulses from this device can shut down areas of the brain that are causing seizures if they occur in that area again (Deep brain stimulation or Neuromodulation).
People with uncontrolled seizures are often able to live fulfilling lives by learning to manage their condition through medication, dietary modification, and lifestyle changes.