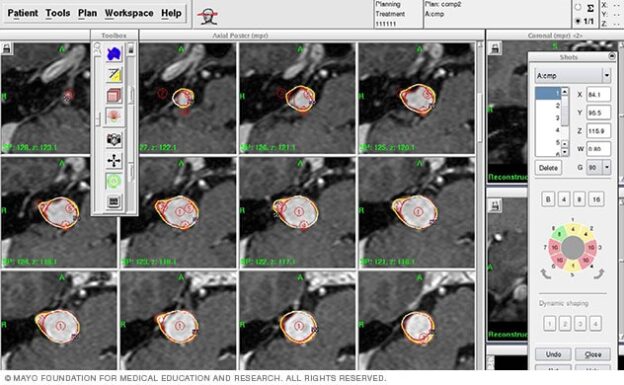
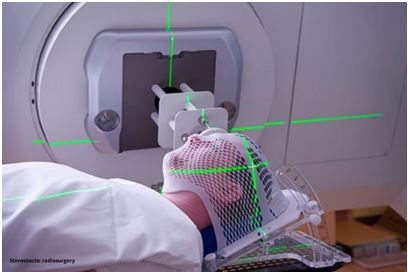
Gamma Knife vs CyberKnife vs LINAC Radiosurgery: Which Is Best?
When patients hear they need treatment for a brain tumor, arteriovenous malformation (AVM), trigeminal neuralgia, or brain metastases, many ask a crucial question: “Which radiosurgery is best—Gamma Knife, CyberKnife, or LINAC?”
Stereotactic radiosurgery (SRS) offers non-invasive brain tumor treatment with sub-millimeter precision—often without open surgery. Yet, the three leading technologies differ in accuracy, treatment sessions, suitability, cost, and availability in India.
This comprehensive, patient-friendly guide compares Gamma Knife vs CyberKnife vs LINAC radiosurgery across indications, accuracy, safety, outcomes, recovery, and cost—helping you make an informed decision with your specialist.
What Is Stereotactic Radiosurgery (SRS)?
Stereotactic radiosurgery (SRS) delivers highly focused radiation to a target in the brain (or spine) with extreme accuracy, sparing surrounding healthy tissue. Despite the name, it involves no incision.
SRS is used for:
- Brain tumors (benign and malignant)
- Brain metastases
- AVMs
- Acoustic neuromas
- Meningiomas
- Trigeminal neuralgia
- Pituitary tumors
- Selected spinal tumors (SBRT)
Authoritative sources like the Mayo Clinic and NIH recognize SRS as a standard, effective option for many intracranial conditions.
Gamma Knife Radiosurgery: An Overview
Gamma Knife radiosurgery is purpose-built for the brain. It uses ~192 cobalt-60 sources that converge precisely on the target.
Key Features
- Designed exclusively for brain conditions
- Exceptional accuracy (sub-millimeter)
- Typically a single-session treatment
- Rigid head frame or frameless options (newer models)
Best Indications
- Brain metastases
- Acoustic neuroma
- Small to medium meningiomas
- AVMs
- Trigeminal neuralgia
Accuracy of Gamma Knife: Among the highest for intracranial targets due to fixed geometry and head immobilization.
CyberKnife Radiosurgery: An Overview
CyberKnife radiosurgery uses a robotic arm with real-time image guidance to deliver radiation from multiple angles.
Key Features
- Robotic, image-guided system
- No rigid head frame (frameless)
- Supports fractionated treatment (multiple sessions)
- Treats brain and spine (SBRT)
Best Indications
- Lesions near critical structures
- Spinal tumors
- Recurrent tumors
- Patients needing fractionation
Accuracy of CyberKnife: Excellent precision with motion tracking, especially useful when fractionation is required.
LINAC-Based Radiosurgery: An Overview
LINAC radiosurgery uses advanced linear accelerators with stereotactic capabilities to deliver SRS or SBRT.
Key Features
- Highly versatile and widely available
- Supports single-session or fractionated SRS
- Advanced imaging and beam shaping
- Brain and spine applications
Best Indications
- Brain tumors and metastases
- Spinal radiosurgery
- When flexibility and availability matter
Accuracy of LINAC radiosurgery: Modern LINACs achieve sub-millimeter accuracy comparable to dedicated systems when properly configured.
Gamma Knife vs CyberKnife vs LINAC: Side-by-Side Comparison
| Feature | Gamma Knife | CyberKnife | LINAC |
|---|
| Primary Use | Brain only | Brain & Spine | Brain & Spine |
| Accuracy | Excellent | Excellent | Excellent (modern) |
| Treatment Sessions | Single session | Single or fractionated | Single or fractionated |
| Immobilization | Frame / Frameless | Frameless | Frameless |
| Spine Treatment | No | Yes | Yes |
Which Radiosurgery Is Best for Brain Tumors?
There is no single “best” system for every patient. The optimal choice depends on:
- Tumor type and size
- Location (near optic nerves, brainstem)
- Need for single-session vs fractionated treatment
- Brain vs spine involvement
General guidance:
- Gamma Knife: Small to medium intracranial lesions needing single-session precision
- CyberKnife: Lesions near critical structures or spine requiring fractionation
- LINAC: Versatile option for brain and spine with modern planning
Safety, Side Effects, and Outcomes
All three technologies have strong safety profiles when used appropriately.
Common side effects:
- Temporary headache or fatigue
- Transient swelling (managed medically)
According to studies indexed on PubMed, local control rates for SRS in brain metastases often exceed 85–90% in selected patients.
Radiosurgery vs Open Brain Surgery vs Radiation Therapy
- Radiosurgery vs open surgery: No incision, shorter recovery, ideal for small/deep lesions
- Radiosurgery vs conventional radiation: Higher precision, fewer sessions, better tissue sparing
Radiosurgery is especially valuable for elderly or high-risk patients.
Cost of Gamma Knife vs CyberKnife vs LINAC in India
Radiosurgery cost in India varies by technology, complexity, and sessions:
- Gamma Knife: Typically single-session, premium technology
- CyberKnife: Cost varies with fractionation
- LINAC: Often more cost-flexible
India offers world-class radiosurgery at a fraction of global costs, making it a preferred destination.
Radiosurgery at Dr. Rao’s Hospital, Guntur
At Dr. Rao’s Hospital, radiosurgery planning and patient selection are led by Dr. Mohana Rao Patibandla, focusing on:
- Evidence-based selection of technology
- Multidisciplinary planning
- Patient-centric outcomes
Explore our Neurosurgery, Neurology, and Spine Surgery services.
Which radiosurgery is safest?
Gamma Knife, CyberKnife, and LINAC radiosurgery are all safe when appropriately selected. Safety depends more on correct indication, planning, and expertise than on the machine itself.
Is radiosurgery painful?
Radiosurgery is generally painless. Most patients return home the same day with minimal discomfort and rapid recovery.
Why choose Dr. Rao’s Hospital for radiosurgery?
At Dr. Rao’s Hospital, led by Dr. Mohana Rao Patibandla, patients receive advanced, ethical, and personalized radiosurgery care.
Consult a Radiosurgery Specialist in Guntur
If you’re searching for the best radiosurgery for brain tumors or expert guidance on Gamma Knife vs CyberKnife vs LINAC, visit Dr. Rao’s Hospital. Dr. Mohana Rao Patibandla is a fellowship trained Radiosurgeon having excellent experience in all the three modalities.
📞 090100 56444
📧 info@drraoshospitals.com
📍 Contact Dr. Rao’s Hospital
Facebook |
Instagram |
YouTube |
LinkedIn |
X (Twitter)
People Also Ask: Radiosurgery Decision-Making
Is Gamma Knife better than CyberKnife for brain tumors?
Gamma Knife is often preferred for small to medium brain tumors requiring single-session treatment with very high precision. CyberKnife may be better when fractionated treatment is needed or when the tumor is close to sensitive brain structures. Both treatments are equally efficacious.
Which radiosurgery is best for tumors near the brainstem or optic nerve?
For tumors near critical structures like the brainstem or optic nerves, fractionated radiosurgery using CyberKnife or LINAC is often safer, as it delivers radiation over multiple sessions to reduce risk to surrounding tissue.
Is LINAC radiosurgery as accurate as Gamma Knife?
Modern LINAC-based radiosurgery systems achieve sub-millimeter accuracy comparable to Gamma Knife when advanced imaging, planning, and immobilization are used by experienced radiosurgery teams.
Can radiosurgery completely cure brain tumors?
Radiosurgery can control or stop growth of many brain tumors, especially benign tumors and metastases. Cure depends on tumor type, size, biology, and response to radiation rather than the machine alone.
Is radiosurgery safe for elderly patients?
Yes. Radiosurgery is particularly suitable for elderly or high-risk patients because it is non-invasive, does not require general anesthesia, and has a short recovery time compared to open brain surgery.
How long does a radiosurgery session take?
Gamma Knife treatment usually takes a few hours in a single session. CyberKnife and LINAC sessions are shorter but may require multiple visits if fractionated treatment is planned.
What is the recovery time after radiosurgery?
Most patients resume normal activities within one to two days after radiosurgery. There are usually no surgical wounds, and hospital stay is minimal or not required.
Does radiosurgery cause hair loss?
Hair loss after radiosurgery is uncommon and usually limited to a small area near the treatment site. It is often temporary and depends on dose and target location.
What are the long-term side effects of radiosurgery?
Long-term side effects are uncommon but may include delayed swelling or radiation-related changes, which are usually manageable with medications and close follow-up.
Is radiosurgery better than conventional radiation therapy?
Radiosurgery is more precise than conventional radiation therapy, delivers higher doses in fewer sessions, and minimizes exposure to healthy brain tissue, making it ideal for small, well-defined targets.
Can radiosurgery be repeated if the tumor comes back?
In selected cases, radiosurgery can be repeated if a tumor recurs or new lesions appear. The decision depends on prior dose, location, and overall brain tolerance.
Is radiosurgery available near me in Andhra Pradesh?
Advanced radiosurgery options are available in Andhra Pradesh at specialized centers. Treatment selection depends on the technology available and the expertise of the treating team.
Who decides which radiosurgery technology I should receive?
The choice of Gamma Knife, CyberKnife, or LINAC is made by a multidisciplinary team based on tumor characteristics, safety considerations, and expected outcomes—not patient preference alone.
Who is a radiosurgery specialist in Guntur?
Radiosurgery evaluation and treatment planning at Dr. Rao’s Hospital is guided by Dr. Mohana Rao Patibandla, with a focus on safe, evidence-based, and patient-specific care.
Need Expert Guidance on Radiosurgery?
If you or your loved one is deciding between Gamma Knife, CyberKnife, or LINAC radiosurgery, expert evaluation is critical to choose the safest and most effective option.
Consult the team at Dr. Rao’s Hospital for personalized radiosurgery planning based on your diagnosis, imaging, and overall health.
📞 090100 56444
📧 info@drraoshospitals.com
📍 Book an Appointment
The best radiosurgery is the one chosen correctly—for you.
Facebook |
Instagram |
YouTube |
LinkedIn |
X (Twitter)
People Also Ask: Advanced Radiosurgery Considerations
Is radiosurgery suitable for large brain tumors?
Radiosurgery is most effective for small to medium-sized brain tumors. Larger tumors may require staged or fractionated radiosurgery, or a combination of surgery and radiosurgery, depending on location and symptoms.
Can radiosurgery treat tumors without a biopsy?
Yes. In many cases, radiosurgery is performed based on characteristic MRI findings, especially for metastases, meningiomas, and acoustic neuromas, without the need for a surgical biopsy.
Is radiosurgery effective for brain metastases?
Radiosurgery is highly effective for brain metastases, offering excellent local control while preserving cognitive function, especially when treating limited numbers of metastatic lesions.
Which radiosurgery is best for acoustic neuroma?
Gamma Knife is commonly preferred for acoustic neuromas due to its high precision and long-term tumor control, while CyberKnife or LINAC may be chosen when fractionation is needed to protect hearing.
Can radiosurgery treat trigeminal neuralgia?
Yes. Radiosurgery is an established, non-invasive treatment for trigeminal neuralgia, providing pain relief in many patients who do not respond to medications or are unfit for surgery.
Is radiosurgery effective for AVMs?
Radiosurgery is effective for small to moderate arteriovenous malformations (AVMs), causing gradual closure of abnormal vessels over months to years while avoiding open brain surgery.
Does radiosurgery affect memory or brain function?
Radiosurgery is designed to minimize impact on healthy brain tissue. When properly planned, it preserves memory and cognitive function better than conventional radiation therapy.
How is treatment accuracy ensured in radiosurgery?
Accuracy is ensured using high-resolution imaging, precise immobilization, computerized treatment planning, and real-time image guidance, achieving sub-millimeter targeting accuracy.
Can radiosurgery be combined with surgery or chemotherapy?
Yes. Radiosurgery is often part of a multimodal treatment plan and may be combined with microsurgery, chemotherapy, immunotherapy, or targeted therapy for optimal outcomes.
Is radiosurgery a one-day procedure?
Most radiosurgery treatments are completed in one day, especially Gamma Knife. Some cases require multiple sessions, but hospitalization is usually not necessary.
What follow-up is needed after radiosurgery?
Follow-up includes periodic MRI scans and clinical evaluations to monitor tumor response and detect delayed effects. Most patients resume normal routines immediately after treatment.
Is radiosurgery available near me in Guntur?
Patients in and around Guntur can access advanced radiosurgery evaluation and treatment planning at specialized centers offering modern SRS technologies. Dr. Rao’s Hospital provides best radiosurgery and radiation plan will be delivered by Dr. Mohana Rao Patibandla.
Who plans radiosurgery treatment?
Radiosurgery planning is done by a multidisciplinary team involving a neurosurgeon, radiation oncologist, and medical physicist to ensure safety, accuracy, and optimal outcomes. Dr. Mohana Rao Patibandla is a radiosurgery fellowship trained neurosurgeon.
Who should not undergo radiosurgery?
Radiosurgery may not be suitable for very large tumors causing severe pressure, certain radiation-resistant tumors, or conditions requiring immediate surgical decompression.
Who is a trusted radiosurgery expert in Guntur?
Radiosurgery evaluation and treatment planning at Dr. Rao’s Hospital is guided by Dr. Mohana Rao Patibandla, focusing on safe, evidence-based, and patient-specific care.
Make the Right Choice in Radiosurgery
Choosing between Gamma Knife, CyberKnife, and LINAC radiosurgery requires expert evaluation—not guesswork.
At Dr. Rao’s Hospital, each patient receives individualized radiosurgery planning based on diagnosis, imaging, safety, and long-term outcomes.
📞 090100 56444
📧 info@drraoshospitals.com
📍 Schedule a Consultation
The best radiosurgery is not the machine—it’s the decision behind it.
Facebook |
Instagram |
YouTube |
LinkedIn |
X (Twitter)
గామా నైఫ్ vs సైబర్నైఫ్ vs లినాక్ రేడియోసర్జరీ: ఏది ఉత్తమం?
మెదడు ట్యూమర్, మెదడుకు వ్యాపించిన క్యాన్సర్, ట్రైజెమినల్ న్యూరాల్జియా లేదా AVM వంటి సమస్యలు వచ్చినప్పుడు చాలా మంది రోగుల కుటుంబాల్లో ఒకే ప్రశ్న వస్తుంది: “గామా నైఫ్ మంచిదా? సైబర్నైఫ్ బెటరా? లేక లినాక్ రేడియోసర్జరీనా?”
ఈ మూడు పద్ధతులు స్టీరియోటాక్టిక్ రేడియోసర్జరీ (SRS) కిందికి వస్తాయి. ఇవి శస్త్రచికిత్స లేకుండా, అత్యంత ఖచ్చితంగా కిరణ చికిత్స ఇవ్వగల ఆధునిక సాంకేతిక పద్ధతులు. కానీ – ప్రతి రోగికి ఒకే పద్ధతి సరిపోదు.
ఈ పూర్తి తెలుగు మార్గదర్శకంలో గామా నైఫ్ vs సైబర్నైఫ్ vs లినాక్ రేడియోసర్జరీ మధ్య తేడాలు, ప్రయోజనాలు, ఉపయోగించే సందర్భాలు, భద్రత, ఫలితాలు అన్నీ సులభంగా తెలుసుకుందాం.
స్టీరియోటాక్టిక్ రేడియోసర్జరీ (SRS) అంటే ఏమిటి?
రేడియోసర్జరీ అంటే నిజానికి “ఆపరేషన్” కాదు. ఇది అత్యంత శక్తివంతమైన కిరణాలను (Radiation)
మెదడులోని ఒక నిర్దిష్ట ప్రాంతంపై అత్యంత ఖచ్చితంగా కేంద్రీకరించి ఆ ట్యూమర్ లేదా అసాధారణ కణాలను నియంత్రించే చికిత్స.
ఇందులో:
- కట్ లేదా కుట్టు ఉండదు
- జనరల్ అనస్థీషియా అవసరం ఉండదు
- చాలా సందర్భాల్లో అదే రోజు ఇంటికి వెళ్లవచ్చు
గామా నైఫ్ రేడియోసర్జరీ అంటే ఏమిటి?
గామా నైఫ్ అనేది ప్రత్యేకంగా మెదడు చికిత్స కోసం మాత్రమే రూపొందించిన రేడియోసర్జరీ పద్ధతి.
ఇది సుమారు 190కి పైగా గామా కిరణాలను ఒకే బిందువుపై కేంద్రీకరిస్తుంది.
గామా నైఫ్ ముఖ్య లక్షణాలు
- మెదడుకు మాత్రమే ఉపయోగిస్తారు
- అత్యంత ఖచ్చితత్వం (sub-millimeter accuracy)
- సాధారణంగా ఒకే సెషన్లో చికిత్స
గామా నైఫ్ ఎక్కువగా ఉపయోగించే పరిస్థితులు
- మెదడు ట్యూమర్లు (చిన్న – మధ్య పరిమాణం)
- అకూస్టిక్ న్యూరోమా
- మెనింజియోమా
- AVM
- ట్రైజెమినల్ న్యూరాల్జియా
👉 ఒకే రోజులో పూర్తయ్యే, అత్యంత ఖచ్చితమైన చికిత్స కావాలంటే గామా నైఫ్ అద్భుతమైన ఎంపిక.
సైబర్నైఫ్ రేడియోసర్జరీ అంటే ఏమిటి?
సైబర్నైఫ్ అనేది రోబోటిక్ టెక్నాలజీతో పనిచేసే రేడియోసర్జరీ పద్ధతి. ఇది కిరణాలను వివిధ కోణాల నుంచి ఇస్తూ ట్యూమర్ కదలికలను కూడా ట్రాక్ చేయగలదు.
సైబర్నైఫ్ ముఖ్య లక్షణాలు
- మెదడు + వెన్నెముకకు ఉపయోగించవచ్చు
- ఫ్రేమ్ అవసరం ఉండదు
- ఒకటి కంటే ఎక్కువ సెషన్లలో చికిత్స (Fractionated)
సైబర్నైఫ్ ఎక్కువగా ఉపయోగించే పరిస్థితులు
- సెన్సిటివ్ నరాలకు దగ్గరగా ఉన్న ట్యూమర్లు
- స్పైనల్ ట్యూమర్లు
- మళ్లీ వచ్చిన ట్యూమర్లు
👉 సున్నితమైన ప్రాంతాల్లో ట్యూమర్ ఉంటే, క్రమంగా కిరణాలు ఇవ్వాలంటే సైబర్నైఫ్ అనుకూలం.
లినాక్ (LINAC) రేడియోసర్జరీ అంటే ఏమిటి?
LINAC (లినియర్ యాక్సిలరేటర్)
అనేది బహుముఖ వినియోగం ఉన్న ఆధునిక రేడియేషన్ యంత్రం. ఇది SRS (మెదడు) మరియు SBRT (స్పైన్) రెండింటికీ ఉపయోగపడుతుంది.
లినాక్ ముఖ్య లక్షణాలు
- మెదడు + వెన్నెముక చికిత్స
- ఒకే సెషన్ లేదా బహుళ సెషన్లు
- అధునాతన ఇమేజింగ్, ప్లానింగ్
👉 సరైన సాంకేతికత మరియు అనుభవం ఉంటే
లినాక్ కూడా గామా నైఫ్ స్థాయిలో ఖచ్చితత్వం ఇస్తుంది.
గామా నైఫ్ vs సైబర్నైఫ్ vs లినాక్ – తేడాలు
| లక్షణం | గామా నైఫ్ | సైబర్నైఫ్ | లినాక్ |
|---|
| మెదడు చికిత్స | అవును | అవును | అవును |
| స్పైన్ చికిత్స | కాదు | అవును | అవును |
| సెషన్లు | ఒకే సెషన్ | బహుళ | ఒకటి / బహుళ |
| ఖచ్చితత్వం | అత్యుత్తమం | అత్యుత్తమం | అత్యుత్తమం (ఆధునిక) |
అయితే… ఏ రేడియోసర్జరీ ఉత్తమం?
ఇదే అత్యంత ముఖ్యమైన విషయం: “ఉత్తమమైన యంత్రం” అనే పదం లేదు – “ఉత్తమంగా ఎంచుకున్న చికిత్స” మాత్రమే ఉంటుంది.
ఎంపిక ఆధారపడేది:
- ట్యూమర్ రకం & పరిమాణం
- మెదడులో ఉన్న స్థానం
- ఒకే సెషన్ అవసరమా లేదా క్రమంగా చికిత్స కావాలా
- రోగి వయసు, ఆరోగ్యం
డా. రావు హాస్పిటల్లో రేడియోసర్జరీ దృక్పథం
డా. రావు హాస్పిటల్ లో యంత్రం కంటే ముందుగా రోగి భద్రత మరియు ఫలితం ముఖ్యం.
రేడియోసర్జరీ ప్లానింగ్ మరియు నిర్ణయాలు Dr. Mohana Rao Patibandla, నాయకత్వంలో న్యూరోసర్జన్, రేడియేషన్ ఆంకాలజిస్ట్, ఫిజిసిస్ట్ బృందం ద్వారా జరుగుతాయి.
ప్రతి రోగికి వ్యక్తిగతంగా సరిపోయే పద్ధతినే ఎంచుకుంటారు.
మీకు ఏ రేడియోసర్జరీ సరిపోతుందో తెలుసుకోవాలా?
మీరు లేదా మీ కుటుంబ సభ్యులు గామా నైఫ్, సైబర్నైఫ్ లేదా లినాక్ రేడియోసర్జరీ గురించి సందిగ్ధంలో ఉంటే, నిపుణుల సలహా తప్పనిసరి.
📞 090100 56444
📧 info@drraoshospitals.com
📍 అపాయింట్మెంట్ కోసం సంప్రదించండి
గుర్తుంచుకోండి: యంత్రం కాదు – సరైన నిర్ణయమే ప్రాణాలు కాపాడుతుంది.
Facebook |
Instagram |
YouTube |
LinkedIn |
X (Twitter)