Arm/leg weakness – The best treatment at Dr Raos hospital, Guntur
Introduction
Arm & Leg Weakness-The human body is a fantastic machine of many different parts that all work together to keep us moving. However, sometimes things can go wrong, and we may experience weakness in one or more of our limbs. This can be caused by several conditions, some of which are more serious than others. This article will examine some of the most common causes of arm or leg weakness and what you can do about them. Many different conditions can cause weakness in the arms or legs. Some common ones include slipped discs, stroke, pinched nerves, peripheral neuropathy, and spinal lesions or tumors. These conditions can cause different symptoms and may require different treatment options. If you are experiencing any arm or leg weakness, it is essential to see a doctor so that they can properly diagnose the underlying cause and recommend the best course of treatment. If looking for arm or leg weakness due to neurological causes, please consult the best neurosurgeon, neurologist, or spine surgeon, Dr. Rao, Dr. Raos hospital, Guntur. Dr. Raos is the best neurosurgery, spine surgery, and neurology hospital in Guntur and Andhra Pradesh. Contact us 90010056444 or 9010057444
Slipped disc
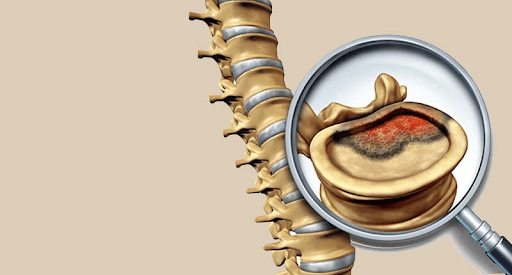
A slipped disc occurs when the gel-like center of a disc ruptures through a weak spot in the tough outer layer. This can happen due to a sudden injury or from the wear and tear of aging. The gel squeezes out and puts pressure on the nearby nerves. This can cause pain, numbness, or weakness in the arm or leg. If you are looking for the best spinal cord tumor disease treatment, visit the best neurosurgery and spine surgery hospital, Dr. Rao’s hospital, with the best neurosurgeon and spine surgeon Dr. Rao.
Stroke
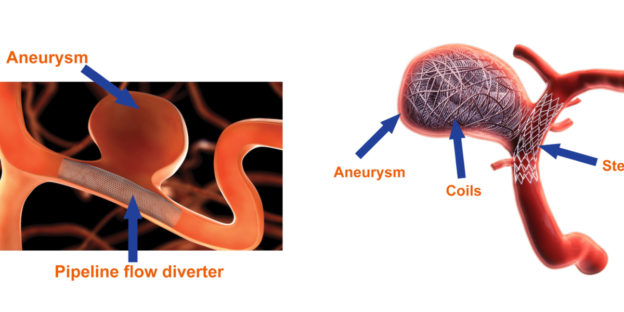
A stroke is a medical emergency. It happens when the blood supply to part of your brain is cut off. A stroke can be caused by a clot blocking the blood vessel or the blood vessel bursting. Stroke symptoms include • Sudden weakness or numbness in your face, arm, or leg, especially on one side of your body • Sudden confusion or trouble speaking • Sudden trouble seeing in one or both eyes • Sudden trouble walking, dizziness, or loss of balance or coordination • Sudden severe headache with no known cause If you have any of these symptoms,
Pinched nerve
A pinched nerve occurs when too much pressure is applied to a nerve by surrounding tissues. This pressure can irritate the nerve and cause pain, tingling, numbness, or weakness. There are many possible causes of a pinched nerve. A herniated disc in the spine can pressure nerves as they exit the spinal column. Poor posture and repetitive motions can also lead to a pinched nerve. Obesity, pregnancy, and even sleeping on your stomach can put extra pressure on nerves and cause them to become irritated. Treating a pinched nerve depends on the underlying cause. If you have a herniated disc, your doctor may recommend physical therapy or surgery to relieve the pressure on the affected nerve. If your pinched nerve is caused by poor posture, you will need to correct your posture and avoid any repetitive motions that may aggravate the nerve. You may also need to lose weight if obesity contributes to your pinched nerve. If you have a pinched nerve, it is essential to seek treatment as soon as possible. Left untreated, a pinched nerve can permanently damage the affected nerve. If you are looking for the best spinal cord tumor disease treatment, visit the best neurosurgery and spine surgery hospital, Dr. Rao’s hospital, with the best neurosurgeon and spine surgeon Dr. Rao.
Peripheral neuropathy
Peripheral neuropathy is a condition in which the nerves that carry messages to and from the brain and spinal cord are damaged. This damage can cause problems with sensation, movement, and other functions. There are many types of peripheral neuropathy, each with its symptoms. Some common symptoms include numbness, tingling, pain, and weakness. These symptoms can occur in any body part, but they are most often felt in the hands and feet. Many things, including diabetes, certain medications, infections, injuries, and exposure to toxins, can cause peripheral neuropathy.
Treatment for peripheral neuropathy depends on the underlying cause. In many cases, the exact cause of the condition is unknown. In some cases, treatment may not be necessary. For example, if the disease is caused by an infection or injury that has healed, the nerve damage may improve over time. In other cases, treatment may be necessary to relieve symptoms and prevent further damage to the nerves. Common treatments include physical therapy, medications, and surgery. If you are looking for the best peripheral neuropathy treatment, visit the best neurology hospital Dr. Rao’s, with the best neurosurgeon Dr. Rao.
Spinal lesion or tumor
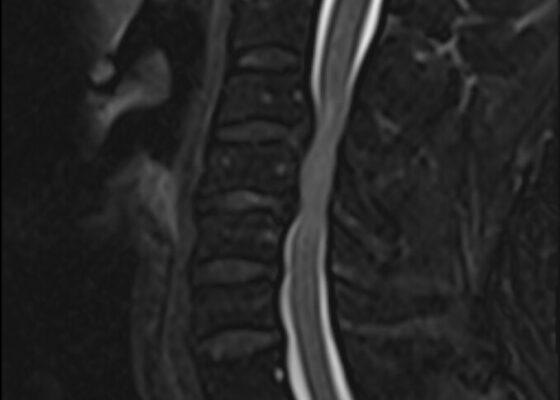
A spinal lesion or tumor can cause arm or leg weakness if it presses on the spinal cord or nerves. The spinal cord is a bundle of nerves that runs from the brain through the spine. Nerves branch off the spinal cord and travel to all body parts. If a lesion or tumor presses on the spinal cord or nerves, it can cause weakness, numbness, or paralysis in the arms or legs. If you are looking for the best spinal cord tumor disease treatment, visit the best neurosurgery and spine surgery hospital, Dr. Rao’s hospital, with the best neurosurgeon and spine surgeon Dr. Rao.
Guillain-Barré Syndrome
Guillain-Barré syndrome (GBS) is a rare but serious autoimmune disorder that affects the peripheral nervous system. The exact cause of GBS is unknown, but it is thought to be triggered by an infection or other immune system disorder. Symptoms of GBS can range from mild to severe and may include muscle weakness, paralysis, and even death. Early diagnosis and treatment of GBS are critical for the best possible outcome.
Symptoms of GBS can range from mild to severe. Early symptoms may include muscle weakness, tingling, or numbness in the extremities. These symptoms can quickly progress to paralysis and may even affect the muscles used for breathing. In some cases, GBS can be fatal. Early diagnosis and treatment are critical for the best possible outcome.
Multiple sclerosis
Multiple sclerosis is a debilitating disease that affects the nervous system. There is no known cure for MS, but treatments available can help manage the symptoms. The two main types of MS are relapsing-remitting MS, and progressive MS. Relapsing-remitting MS is the most common type of MS. It is characterized by periods of remission, during which symptoms improve or disappear, followed by periods of relapse, during which symptoms worsen. Progressive MS is a less common type of MS. It is characterized by a gradual worsening of symptoms, with no periods of remission. Multiple sclerosis is a debilitating disease that affects the nervous system. There is no known cure for MS, but treatments available can help manage the symptoms. The two main types of MS are relapsing-remitting MS and progressive MS. Looking for the best Multiple sclerosis disease treatment, visit the best neurology hospital, Dr. Rao’s hospital, with the best neurosurgeon Dr. Rao.
Parkinson’s disease
Parkinson’s disease is a degenerative disorder of the central nervous system that often impairs a person’s motor skills, speech, and other functions. The disease is caused by the death of nerve cells in the brain that produce dopamine, a chemical that helps regulate movement.
There are two main types of Parkinson’s disease: early-onset and late-onset. Early-onset Parkinson’s disease usually affects people under the age of 50, while late-onset Parkinson’s disease typically affects people over the age of 60.
There is no cure for Parkinson’s disease, but there are treatments that can help improve a person’s quality of life.
Early-onset Parkinson’s disease is the less common type, accounting for about 10 percent of all cases. The average age of onset is around 47 years old. Men are more likely to develop early-onset Parkinson’s disease than women.
The symptoms of early-onset Parkinson’s disease are similar to those of late-onset Parkinson’s but tend to be more severe. People with early-onset Parkinson’s disease may have difficulty walking and talking and may also experience tremors, rigidity, and problems with balance.
There is no cure for early-onset Parkinson’s disease, but there are treatments that can help improve a person’s quality of life. Medications can help relieve symptoms, and surgery may be an option for some people.
Late-onset Parkinson’s disease is the more common type, accounting for about 90 percent of all cases. The average age of onset is around 60 years old. Men and women are equally likely to develop late-onset Parkinson’s disease.
The symptoms of late-onset Parkinson’s disease are similar to those of early-onset Parkinson’s disease but tend to be less severe. People with late-onset Parkinson’s disease may have difficulty walking and talking and may also experience tremors, rigidity, and problems with balance.
There is no cure for late-onset Parkinson’s disease, but there are treatments that can help improve a person’s quality of life. Medications can help relieve symptoms, and surgery may be an option for some people.
Parkinson’s disease is a degenerative disorder of the central nervous system that often impairs a person’s motor skills, speech, and other functions. The disease is caused by the death of nerve cells in the brain that produce dopamine, a chemical that helps regulate movement. There is no cure for Parkinson’s disease, but there are treatments that can help improve a person’s quality of life. If you are looking for the best Parkinson’s disease treatment, visit the best neurology hospital, Dr. Rao’s, with the best neurosurgeon Dr. Rao.
Myasthenia gravis (MG)
Myasthenia gravis (MG) is a chronic autoimmune neuromuscular disease that is characterized by varying degrees of skeletal muscle weakness. The predominant symptom of MG is muscle weakness that increases during periods of activity and improves with rest.
There are two main types of MG: generalized MG (gMG) and ocular MG (oMG). gMG is the more common form of the disease, affecting both men and women of all ages. oMG is a less common form of MG that primarily affects women under 40.
There is no cure for MG, but treatments are available to help manage the symptoms.
Generalized MG
gMG is the more common form of MG, affecting men and women of all ages. The symptoms of gMG can vary from mild to severe, and they may come and go. The most common symptom of gMG is muscle weakness that increases during periods of activity and improves with rest.
Other symptoms of gMG may include:
• Fatigue
• Muscle cramps
• Difficulty speaking
• Difficulty swallowing
• Shortness of breath
• blurred vision
gMG is typically diagnosed based on muscle weakness and other characteristic symptoms. A variety of tests may be used to confirm the diagnosis, including:
• Blood tests
• Muscle biopsy
• Edrophonium test
• Tensilon test
There is no cure for gMG, but treatments are available to help manage the symptoms. Treatment options may include:
• Medications
• Surgery
• Plasma exchange
• Immunotherapy
Ocular MG
oMG is a less common form of MG, primarily affecting women under 40. The symptoms of oMG are typically milder than those of gMG, and they tend to be limited to the muscles around the eyes.
The most common symptom of oMG is muscle weakness that causes drooping of the eyelids (ptosis). Other symptoms of oMG may include:
• Diplopia
• Difficulty moving the eyes
• Muscle weakness in the face
oMG is typically diagnosed based on muscle weakness and other characteristic symptoms. A variety of tests may be used to confirm the diagnosis, including:
• Blood tests
• Muscle biopsy
• Edrophonium test
• Tensilon test
There is no cure for oMG, but treatments are available to help manage the symptoms. Treatment options may include:
• Medications
• Surgery
• Plasma exchange
• Immunotherapy
Myasthenia gravis (MG) is a chronic autoimmune neuromuscular disease characterized by varying skeletal muscle weakness. There are two main types of MG: generalized MG (gMG) and ocular MG (oMG). gMG is the more common form of the disease, affecting men and women of all ages. oMG is a less common form of MG, primarily affecting women under 40. There is no cure for MG, but treatments are available to help manage the symptoms. If you are looking for the best Myasthenia Gravis disease treatment, visit the best neurology hospital Dr. Rao’s, with the best neurosurgeon Dr. Rao.
Amyotrophic lateral sclerosis, or ALS
Amyotrophic lateral sclerosis, or ALS, is a progressive neurodegenerative disease that affects nerve cells in the brain and the spinal cord. The disease is characterized by muscle weakness and paralysis, and it can eventually lead to death.
There is no known cure for ALS, but there are treatments that can help to improve quality of life and extend life expectancy. The most important thing for people with ALS is to get an early diagnosis and to start treatment as soon as possible.
Early Diagnosis and Treatment
Early diagnosis and treatment of ALS are essential for the best possible outcome. The sooner the disease is diagnosed, the sooner treatment can begin. Some different therapies are available for ALS, and the best course of treatment will vary from person to person.
Some of the most common treatments for ALS include physical therapy, occupational therapy, speech therapy, and respiratory therapy. These therapies can help to improve quality of life and extend life expectancy. In some cases, medications may also be prescribed to help manage symptoms.
Clinical Trials
Clinical trials are an essential part of the search for a cure for ALS. These trials test new treatments and therapies to see if they are safe and effective. Participation in a clinical trial can be a great way to help researchers find a cure for ALS.
Clinical trials are an essential part of the fight against ALS, and we need your help to find a cure. There are several clinical trials currently underway for ALS. If you are interested in participating in a clinical trial, talk to your doctor about your options.
ALS is a progressive neurodegenerative disease that affects nerve cells in the brain and the spinal cord. The condition is characterized by muscle weakness and paralysis, which can eventually lead to death. There is no known cure for ALS, but there are treatments that can help to improve quality of life and extend life expectancy. The most important thing for people with ALS is to get an early diagnosis and to start treatment as soon as possible. If you are looking for the best ALS, Amyotrophic lateral sclerosis, or motor neuron disease treatment, visit the best neurology hospital, Dr. Rao’s hospital, with the best neurosurgeon Dr. Rao.
Conclusion
In conclusion, there are many potential causes of arm or leg weakness. Some common causes include slipped discs, strokes, pinched nerves, and peripheral neuropathy. However, there are also less common causes, such as spinal lesions or tumors. If you are experiencing arm or leg weakness, you must see a doctor to diagnose and treat the cause properly. If looking for arm or leg weakness due to neurological causes, please consult the best neurosurgeon, neurologist, or spine surgeon, Dr. Rao, Dr. Raos hospital, Guntur. Dr. Raos is the best neurosurgery, spine surgery, and neurology hospital in Guntur and Andhra Pradesh. Contact us 90010056444 or 9010057444