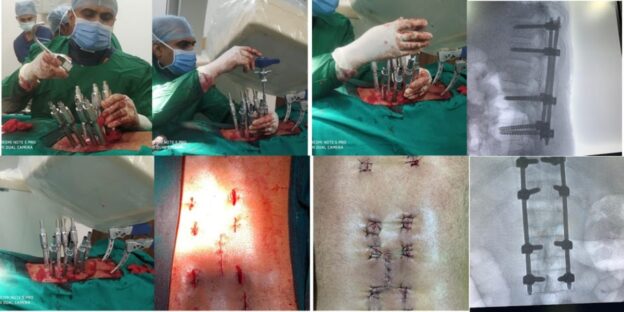
Minimally Invasive Spine Surgery: A Gateway to Pain-Free Living
Are you seeking relief from spine-related discomfort? Look no further than Dr. Rao’s Hospital, your advanced and effective spine care destination. Led by the eminent Dr. Rao, a renowned neurosurgeon, our hospital is committed to providing top-notch treatments, including minimally invasive spine surgery, to enhance your quality of life.
Back and neck pain can be life-disrupting. If medications and physiotherapy haven’t helped, minimally invasive spine surgery (MISS) can relieve nerve compression with tiny incisions, less pain, and faster recovery. At Dr. Rao’s Hospital—the top spine hospital in Guntur—Dr. Mohana Rao Patibandla performs endoscopic, keyhole, and microsurgical procedures tailored to herniated discs, spinal stenosis, spondylolisthesis, and degenerative disc disease. This guide explains the types of MISS, candidacy, benefits, recovery timelines, and costs in Guntur & Andhra Pradesh.
What Is Minimally Invasive Spine Surgery?
MISS uses tubular retractors, endoscopes, or microscopes through 8–20 mm incisions to reach the spine without cutting through large muscle planes. By preserving muscles and ligaments, MISS reduces blood loss, post-operative pain, infection risk, and hospital stay. Many procedures are now outpatient spine surgery with same-day discharge.
Common goals include decompressing pinched nerves, removing herniated disc fragments, and stabilizing segments with minimally invasive lumbar fusion when needed. (Background reading: Mayo Clinic)
Procedures We Offer in Guntur (Tailored to Your Diagnosis)
Endoscopic Discectomy (Keyhole)
Best for herniated discs and select spinal stenosis. Using a 7–8 mm endoscope, Dr. Rao removes the offending disc fragment through a tiny incision. Many patients walk the same day. Ideal for those seeking endoscopic spine surgery in Andhra Pradesh with rapid return to work.
Microdiscectomy
The gold standard for radiculopathy from a lumbar disc. Under high-magnification microscopy, a small window relieves nerve pressure while preserving stabilizing structures. Ask about microdiscectomy recovery time (Dr Rao Guntur) during consultation.
Minimally Invasive Decompression (Micro-Laminectomy/Foraminotomy)
For spinal stenosis, we enlarge the canal/foramen via keyhole access to restore space for nerves—frequently done as same-day spine surgery.
Minimally Invasive Fusion
- TLIF (Transforaminal Lumbar Interbody Fusion)—stabilizes slipped segments; reduces back/leg pain.
- LLIF (Lateral Lumbar Interbody Fusion)—side approach to insert a large graft with minimal posterior muscle trauma.
- Percutaneous Pedicle Screws—stabilization via skin punctures, less muscle damage.
Special Programs
- Robotic spine surgery (Guntur)—sub-millimetre accuracy for complex instrumentation.
- Pediatric minimally invasive spine surgery—for select deformities and pars lesions.
- Laser-assisted discectomy—in carefully chosen cases; Dr. Rao will discuss indications and alternatives.
Learn more on our Spine Surgery page and Neurosurgery Department overview.
Minimally Invasive vs Open Spine Surgery
| Feature | MISS (Keyhole/Endoscopic) | Traditional Open |
|---|
| Incision size | 8–20 mm (often single portal) | 15–30 cm or more |
| Muscle dissection | Minimal (muscle-splitting) | Extensive detachment |
| Blood loss | Low | Moderate–High |
| Hospital stay | Day care to 1–2 days | 5 – 7 days (typical) |
| Pain & recovery | Less pain, faster recovery | More pain, longer recovery |
| Return to work | 1–3 weeks (procedure-dependent) | 4–8+ weeks |
[Reference: PubMed – Outcomes of Minimally Invasive vs Open Spine Surgery]
Who Is a Candidate for Minimally Invasive Spine Surgery?
You may be a candidate if you have:
- Herniated disc with sciatica or arm pain failing conservative care
- Spinal stenosis with walking intolerance or neurogenic claudication
- Spondylolisthesis/instability needing fusion (TLIF/LLIF)
- Recurrent disc herniation or foraminal stenosis
During your visit to Dr. Rao’s Hospital, we review MRI, neurological exam, and prior treatments to confirm if minimally invasive back surgery is right for you. Some complex deformities, infections, or tumors may still require open approaches for safety.
Benefits Patients Notice (Why Choose MISS)
- Faster recovery: Early walking; many resume desk work in 1–3 weeks.
- Less pain & blood loss: Reduced tissue trauma and anaesthetic requirements.
- Smaller scars: Better cosmesis and lower wound complications.
- Lower infection risk: Shorter exposure and hospital stay.
- High success rates: Comparable to open surgery in carefully selected cases.
(General context: NIH – Evidence on Minimally Invasive Techniques)
Procedures in Detail (Dr. Rao’s Techniques)
Endoscopic Discectomy at Dr. Rao’s Hospital
Through an 8 mm portal, the endoscope visualizes the disc and nerve. Saline irrigation keeps the view clear. The herniated fragment is removed precisely, decompressing the nerve root. Most patients walk within hours and go home the same day. This is our popular endoscopic discectomy (Guntur) program for working professionals.
Microdiscectomy by Dr. Mohana Rao Patibandla
Using a microscope, a tiny laminotomy is created, the nerve gently mobilized, and the fragment extracted. Indicated for large paracentral herniations causing severe sciatica. Ask about microdiscectomy recovery time (Dr Rao – Guntur).
TLIF & LLIF Fusion (Stabilization)
TLIF places a cage and bone graft after cleaning disc space via a small posterior window; LLIF approaches from the side, allowing a larger graft for indirect decompression. Both use percutaneous screws to minimize muscle damage. Ideal for instability with back/leg pain and for degenerative disc disease surgery (Guntur).
Robotic & Navigation-Assisted Spine Surgery
Robotics can aid screw placement accuracy, reduce radiation, and shorten operative time—especially in complex multi-level cases. Dr. Rao uses navigation to enhance precision for spine fusion surgery (Guntur).
Recovery Timeline: What to Expect After MISS
Day 0–1 (Hospital)
- Mobilization within hours; discharge same day or next morning.
- Oral pain relief; wound care education.
- Physiotherapist teaches safe log-rolling, sitting, and walking.
Week 1–2
- Short walks 3–5 times/day; avoid bending/twisting/heavy lifting.
- Desk work in 7–14 days (procedure-dependent).
- Shower after 48–72 hours if wound is dry.
Week 3–6
- Increase walking distance; begin core activation exercises.
- Driving after 2–4 weeks when pain-free and off sedatives.
- Light yoga or stationery cycling if advised.
Week 6–12
- Gradual return to full activity; sport-specific rehab for athletes.
- Fusion cases (TLIF/LLIF) follow a slower curve; imaging checks integration.
For program details, see Neurology Services and Spine Surgery recovery resources. (General recovery data: Mayo Clinic)
Cost, Insurance & Value in Guntur
The cost of minimally invasive spine surgery in Guntur varies by procedure (endoscopic discectomy, TLIF/LLIF), implants, hospital stay, and insurance coverage. Our team provides transparent estimates and cashless facilitation when possible. MISS can be cost-effective due to shorter admissions, quicker return to work, and fewer wound complications.
For a personalized quote, contact us via the Contact page or call the hospital directly.
Safety & Success Rates
Is minimally invasive spine surgery safe? In experienced hands, yes. Complication rates are similar or lower than open surgery for indicated cases, with faster recovery. Success depends on diagnosis, imaging correlation, surgical expertise, and rehabilitation adherence.
Global literature supports MISS outcomes comparable to open surgery for discectomy and stenosis, with reduced morbidity. [Context: WHO, PubMed]
Why Choose Dr. Rao’s Hospital (Guntur) for MISS?
- Top endoscopic spine surgeon: Dr. Mohana Rao Patibandla—US-trained; extensive MISS portfolio.
- Comprehensive spectrum: Endoscopic discectomy, microdiscectomy, TLIF, LLIF, percutaneous screws, robotic assistance.
- Enhanced recovery: Same-day ambulation, evidence-based pain control, structured rehab.
- Patient-centric care: Clear counselling, transparent costs, outcome tracking.
Explore our Neurosurgery Department and Spine Surgery pages, or learn about the surgeon here.
Frequently Asked Questions About MISS
What symptoms suggest I might need MISS?
Leg or arm pain from a herniated disc, numbness/tingling, weakness, neurogenic claudication (leg heaviness while walking), or persistent back pain with radiological compression often respond well to MISS.
How do I prepare?
Bring prior MRIs, list of medications, and comorbidity details (diabetes, BP). Stop smoking, optimize sugars (HbA1c), and practice prehab exercises if advised.
Will I need fusion?
Only if instability, high-grade spondylolisthesis, or recurrent stenosis warrants it. Otherwise, decompression or discectomy alone may suffice.
When can I return to work?
Desk work often in 1–3 weeks (discectomy/decompression). Fusion (TLIF/LLIF) patients may need 4–8+ weeks, guided by healing and the job’s physical demands.
If you’re searching for the best minimally invasive spine surgeon in Guntur or need a second opinion, visit Dr. Rao’s Hospital. Book your consultation with Dr. Mohana Rao Patibandla today. Contact us at 📞 090100 56444 or 📧 info@drraoshospitals.com.
What are the symptoms of spinal stenosis or a herniated disc?
Common symptoms include back or neck pain radiating to the arm/leg, numbness, tingling, electric-shock pain on coughing or sneezing, and walking intolerance (heaviness in legs). If symptoms persist despite rest, consult our Spine Surgery team.
How is a herniated disc or stenosis diagnosed?
Diagnosis includes clinical examination and MRI/CT scans to locate the compression. We correlate imaging with your symptoms and neurological findings to decide between endoscopic discectomy, microdecompression, or fusion if instability exists. Learn more at our Neurosurgery Department.
Why choose Dr. Rao’s Hospital for minimally invasive spine surgery?
At Dr. Rao’s Hospital, led by Dr. Mohana Rao Patibandla, one of the best neurosurgeons in Guntur, patients receive advanced, compassionate care using cutting-edge minimally invasive and endoscopic spine techniques with fast-track recovery.
Trusted Sources
Quick Links
Follow Dr. Rao’s Hospital
Conclusion: Your Pathway to Pain-Free Living
Living with chronic back or neck pain doesn’t have to be your reality. With today’s technological advancements, minimally invasive spine surgery (MISS) has become the gold standard for treating complex spine disorders with greater precision, safety, and faster recovery. At Dr. Rao’s Hospital in Guntur, Dr. Mohana Rao Patibandla—a top endoscopic and minimally invasive spine surgeon in Andhra Pradesh—offers world-class expertise backed by years of international training and innovation.
Whether you need a microdiscectomy for a herniated disc, endoscopic decompression for spinal stenosis, or TLIF/LLIF for spine stabilization, our mission is to restore your mobility, relieve pain, and help you return to an active life—safely and swiftly.
Visit the Spine Surgery department to learn more about robotic, laser, and keyhole spine surgery options at Dr. Rao’s Hospital.
✨ Why Patients Choose Dr. Rao’s Hospital for Spine Surgery in Guntur
- Led by Dr. Mohana Rao Patibandla—renowned for excellence in minimally invasive neurosurgery.
- State-of-the-art operation theatres equipped for endoscopic and robotic spine surgery.
- Shorter hospital stay and faster discharge for working professionals.
- Comprehensive multidisciplinary team for pain management, physiotherapy, and rehabilitation.
- Transparent costs and ethical medical care.
Patients from across Andhra Pradesh, Telangana, and South India visit Dr. Rao’s Hospital for advanced spine and neurosurgical treatments.
⭐ Patient Experience Highlight
“After suffering severe back pain for months, I underwent an endoscopic discectomy at Dr. Rao’s Hospital. Within two days, I was walking pain-free. Dr. Mohana Rao and his team were compassionate and professional throughout. Highly recommend their expertise!” – Mr. Srinivas, Guntur
Read more patient success stories on our Testimonials page.
📞 Book Your Consultation Today
Take the first step towards a pain-free spine. Schedule an appointment with Dr. Mohana Rao Patibandla—the best minimally invasive spine surgeon in Guntur—and discover your options for modern, safe, and effective spine care.
Contact Us:
📍 Dr. Rao’s Hospital, 12-19-67, Old Bank Road, Kothapet, Guntur, Andhra Pradesh
📞 090100 56444
📧 info@drraoshospitals.com
Visit drraoshospitals.com to explore our Neurosurgery and Spine Surgery specialties.
🧩 Quick Recap of Key Points
- What is MISS? – Keyhole spine surgery using endoscopic or microscopic tools for precision and minimal trauma.
- Who benefits? – Patients with herniated disc, spinal stenosis, spondylolisthesis, or nerve compression.
- Why choose MISS? – Less pain, faster healing, smaller scars, and early mobility.
- Where to get treated? – Dr. Rao’s Hospital, Guntur, led by Dr. Mohana Rao Patibandla.
🧠 Related Blog Articles You May Like
🔗 External References
📲 Stay Connected with Dr. Rao’s Hospital
Final Thoughts
Minimally invasive spine surgery represents not just a medical innovation, but a profound shift in patient recovery and quality of life. Whether you’re struggling with a herniated disc, spinal stenosis, or degenerative changes, Dr. Rao’s Hospital in Guntur offers advanced, compassionate, and evidence-based care to help you reclaim your comfort and mobility.
Let your journey toward a pain-free spine begin today. Trust Dr. Mohana Rao Patibandla—a pioneer in minimally invasive spine surgery in Andhra Pradesh—to deliver precision, safety, and long-term results.
Minimally Invasive Spine Surgery: Benefits & Recovery Expectations
Chronic back pain, sciatica, and spine-related nerve problems can severely affect quality of life. Traditionally, spine surgery involved large incisions, muscle damage, and prolonged recovery. Today, minimally invasive spine surgery has transformed spinal care by offering effective relief with less pain, faster recovery, and smaller incisions.
This comprehensive guide explains the benefits of minimally invasive spine surgery, who is an ideal candidate, and realistic recovery time expectations. It is especially useful for patients searching for endoscopic spine surgery in India, keyhole spine surgery in Guntur, and expert care at a top spine hospital in Andhra Pradesh.
At Dr. Rao’s Hospital, advanced spine care is led by Dr. Mohana Rao Patibandla, a highly experienced neurosurgeon and spine expert known for complex and minimally invasive spine procedures.
What Is Minimally Invasive Spine Surgery?
Minimally invasive spine surgery (MISS) refers to surgical techniques that treat spinal disorders through very small incisions using specialized instruments, microscopes, or endoscopes. Instead of cutting muscles, surgeons gently separate them, preserving normal anatomy.
These techniques are widely used for:
- Herniated disc (slip disc)
- Spinal stenosis
- Sciatica and nerve compression
- Degenerative spine disorders
- Selected spinal fusion cases
MISS is now considered the gold standard for many spine conditions.
Key Benefits of Minimally Invasive Spine Surgery
The advantages of minimally invasive techniques over traditional open surgery are significant.
1. Smaller Incisions & Less Tissue Damage
Spine surgery small incision recovery means minimal muscle injury, leading to less post-operative pain and faster healing.
2. Less Pain After Surgery
Patients experience less pain spine surgery recovery, often requiring fewer pain medications.
3. Faster Recovery & Early Mobilization
Most patients walk within hours or the next day, enabling faster recovery spine surgery.
4. Reduced Blood Loss & Infection Risk
Smaller incisions significantly lower complications.
5. Shorter Hospital Stay
Many patients are discharged within 24–72 hours.
Source: Mayo Clinic
Endoscopic & Keyhole Spine Surgery in Guntur
Endoscopic spine surgery in India, also known as keyhole spine surgery, is one of the most advanced forms of MISS. It uses a high-definition camera inserted through an incision as small as 8–10 mm.
At Dr. Rao’s Hospital spine care unit, endoscopic techniques are used for:
- Endoscopic discectomy in Guntur
- Foraminotomy and decompression
- Sciatica minimally invasive relief
These procedures allow precise nerve decompression with minimal disruption.
Conditions Treated with Minimally Invasive Spine Surgery
Herniated Disc
Herniated disc minimally invasive surgery relieves nerve compression and leg pain with rapid recovery.
Spinal Stenosis
Spinal stenosis minimally invasive treatment involves targeted decompression without destabilizing the spine.
Degenerative Disc Disease
Stabilization or decompression using MISS techniques reduces chronic back pain.
Spinal Fusion
Spinal fusion minimally invasive advantages include less blood loss, smaller scars, and faster rehabilitation.
Scoliosis
Scoliosis correction minimally invasive in Guntur is possible in selected adult cases.
Recovery Timeline: What Patients Can Expect
Minimally invasive spine surgery recovery time depends on procedure type and patient health.
Desk Jobs
- Light work: 1–2 weeks
- Full-time work: 2–4 weeks
Moderate Physical Work
Heavy Labor / Agriculture
- Return: 6–12 weeks with precautions
These timelines are much shorter than conventional surgery.
Why Choose Dr. Rao’s Hospital for Minimally Invasive Spine Surgery?
- Led by Dr Mohana Rao Patibandla, renowned spine expert
- Advanced endoscopic and microscopic spine technology
- High success rates with patient-centric care
- Trusted Dr Rao’s Hospital reviews for spine surgery
This makes it one of the best minimally invasive spine surgery centers in Vijayawada–Guntur region.
Explore Spine Surgery and Neurosurgery Department.
Affordability & Value of Minimally Invasive Spine Surgery in India
Affordable minimally invasive spine surgery in India offers world-class outcomes at a fraction of international costs.
Though initial costs may seem higher, faster recovery and reduced complications lower overall expenses.
Frequently Asked Questions
What are the benefits of minimally invasive spine surgery?
Benefits include smaller incisions, less pain, faster recovery, reduced blood loss, and shorter hospital stay.
How long does recovery take after minimally invasive spine surgery?
Most patients resume daily activities within weeks, much faster than traditional open surgery.
Why choose Dr. Rao’s Hospital for spine surgery?
At Dr. Rao’s Hospital, led by Dr. Mohana Rao Patibandla, one of the best spine surgeons in Guntur, patients receive advanced minimally invasive spine care with excellent outcomes.
Call to Action: If chronic back pain or sciatica is limiting your life, expert help is available.
For consultation with the best spine surgeon in Guntur and advanced minimally invasive spine surgery in Andhra Pradesh, visit Dr. Rao’s Hospital.
📞 090100 56444
📧 info@drraoshospitals.com
📍 Contact Dr. Rao’s Hospital
Facebook | Instagram | YouTube | LinkedIn | X (Twitter) | Google Maps
Technological Edge Behind Modern Minimally Invasive Spine Surgery
The success of minimally invasive spine surgery is closely linked to technology. Over the last decade, rapid advancements have allowed surgeons to operate with extraordinary precision while minimizing tissue trauma.
- High-definition endoscopes: Provide magnified visualization of nerves and discs through tiny incisions.
- Operating microscopes: Enhance accuracy during keyhole decompressions and fusions.
- Image-guided navigation: Ensures correct level identification and implant placement.
- Intraoperative neuromonitoring: Protects spinal cord and nerve roots during surgery.
At Dr. Rao’s Hospital spine care unit, these technologies are integrated into routine practice, allowing safer surgeries even in complex cases.
How Minimally Invasive Surgery Preserves Spinal Stability
A major concern for patients is whether smaller surgeries compromise long-term spine strength. In fact, minimally invasive approaches often preserve stability better than open surgery.
- Natural ligaments are preserved
- Muscle attachments remain intact
- Targeted bone removal avoids unnecessary weakening
This preservation translates into reduced post-operative pain and lower risk of adjacent segment degeneration.
Patient Selection: Who Benefits the Most?
Not every spine condition requires surgery, and not every surgery must be minimally invasive. Careful patient selection is essential.
Ideal candidates include patients with:
- Single or two-level disc herniation
- Localized spinal stenosis
- Sciatica unresponsive to conservative treatment
- Degenerative conditions without severe deformity
A thorough evaluation by a spine specialist near Guntur ensures the right approach is chosen.
Minimally Invasive Spine Surgery vs Conservative Treatment
Patients often ask whether surgery can be avoided entirely. In many cases, conservative care is tried first.
| Treatment | Role | Outcome |
|---|
| Physiotherapy | First-line for most back pain | Improves mobility and strength |
| Medications | Pain and inflammation control | Symptomatic relief |
| Injections | Temporary nerve pain relief | Short-term benefit |
| MISS | Definitive treatment for structural problems | Long-term relief |
Surgery is recommended when structural compression causes persistent pain or neurological deficits.
Role of Endoscopic Spine Surgery in Sciatica Relief
Sciatica minimally invasive relief is one of the most successful applications of endoscopic techniques.
- Direct removal of disc fragments
- Minimal nerve handling
- Immediate leg pain relief in many cases
Patients often report dramatic improvement within days, making endoscopic discectomy a preferred option.
Minimally Invasive Lumbar Decompression: Long-Term Results
Lumbar decompression surgery benefits extend beyond pain relief.
- Improved walking distance
- Better posture and balance
- Reduced dependency on pain medications
Studies show durable outcomes when decompression is performed before severe nerve damage occurs.
Source: PubMed
Minimally Invasive Spinal Fusion: Myths and Reality
Spinal fusion often raises anxiety. Minimally invasive techniques have changed this perception.
- Smaller incisions reduce muscle injury
- Percutaneous screws minimize blood loss
- Earlier mobilization compared to open fusion
Spinal fusion minimally invasive advantages include faster rehabilitation and reduced hospital stay.
Post-Operative Care: The First 6 Weeks
Recovery after MISS follows a structured plan.
Week 1–2
- Walking encouraged
- Basic daily activities allowed
- Wound care and pain control
Week 3–6
- Physiotherapy initiation
- Gradual return to work
- Posture and ergonomics training
Adherence to guidance ensures optimal healing.
Return to Work & Lifestyle After MISS
One of the biggest advantages is early return to normal life.
- Office workers: 2–4 weeks
- Drivers and shop owners: 4–6 weeks
- Manual laborers/agriculture: 8–12 weeks
Customized advice is provided based on occupation.
Long-Term Spine Health After Surgery
Surgery corrects the problem, but long-term success depends on lifestyle.
- Maintain healthy weight
- Strengthen core muscles
- Avoid prolonged bending and poor posture
Patients who follow these principles enjoy sustained relief.
Complication Rates: Minimally Invasive vs Open Surgery
Multiple studies have shown:
- Lower infection rates
- Reduced blood transfusion needs
- Shorter ICU and hospital stays
These findings support the growing global preference for MISS.
Source: NIH
Why Experience Matters in Minimally Invasive Spine Surgery
MISS has a learning curve. Outcomes are directly related to surgeon expertise.
- Accurate patient selection
- Mastery of endoscopic anatomy
- Ability to convert safely if required
This is why choosing a best minimally invasive spine surgeon in Guntur is critical.
Dr. Rao’s Hospital: A Center of Excellence for MISS
Dr Rao’s Hospital reviews for spine surgery consistently highlight:
- Clear communication and counseling
- Advanced technology and safety
- Excellent functional recovery
The hospital has emerged as a top spine hospital in Guntur, India, serving patients from across Andhra Pradesh.
Future of Minimally Invasive Spine Surgery
The future points toward even less invasive solutions.
- Day-care spine surgeries
- Robotic-assisted spine procedures
- AI-guided surgical planning
These innovations aim to further reduce recovery time and improve precision.
Key Takeaways for Patients
- Minimally invasive spine surgery offers faster recovery with less pain
- Not all back pain requires surgery, but structural problems often do
- Expert evaluation ensures the right treatment at the right time
Final Word
Minimally invasive spine surgery represents a major advancement in spinal care—combining science, technology, and surgical expertise to restore mobility and quality of life.
If back pain, sciatica, or spinal nerve compression is affecting your daily activities, modern solutions are available that do not require prolonged suffering or long hospital stays.
Early consultation, expert hands, and advanced technology make all the difference.
Call to Action: If chronic back pain or sciatica is limiting your life, expert help is available.
For consultation with the best spine surgeon in Guntur and advanced minimally invasive spine surgery in Andhra Pradesh, visit Dr. Rao’s Hospital.
📞 090100 56444
📧 info@drraoshospitals.com
📍 Contact Dr. Rao’s Hospital
Facebook | Instagram | YouTube | LinkedIn | X (Twitter) | Google Maps
Real-World Patient Scenarios: How MISS Changes Outcomes
Understanding how minimally invasive spine surgery (MISS) works in real life helps patients make confident decisions. Below are common scenarios seen in daily practice.
Scenario 1: Young Professional With Sciatica
A 32-year-old software engineer with severe leg pain due to lumbar disc herniation failed physiotherapy and medications. Endoscopic discectomy relieved pain within 48 hours, allowing a return to desk work in two weeks—without long-term restrictions.
Scenario 2: Elderly Patient With Spinal Stenosis
A 68-year-old farmer with walking difficulty and leg numbness underwent minimally invasive lumbar decompression. Reduced blood loss and early mobilization minimized complications, restoring walking endurance within weeks.
Scenario 3: Manual Laborer With Recurrent Back Pain
A construction worker with recurrent disc prolapse benefited from keyhole spine surgery, avoiding prolonged hospital stay and enabling graded return to physical work with spine-protection strategies.
Minimally Invasive Spine Surgery in Elderly Patients
Age alone is not a contraindication for surgery. In fact, MISS offers unique advantages for elderly patients.
- Lower anesthesia-related stress
- Reduced blood loss
- Lower infection risk
- Faster mobilization prevents complications like pneumonia or clots
Careful preoperative assessment ensures safety and good outcomes.
MISS for Patients With Diabetes, Hypertension & Comorbidities
Patients with medical comorbidities often fear surgery. Minimally invasive approaches significantly reduce surgical stress.
- Shorter operative time
- Smaller wounds aid faster healing
- Better blood sugar and blood pressure control post-op
This makes MISS particularly suitable for patients with controlled chronic conditions.
Psychological Impact of Faster Recovery
Recovery is not only physical—it is psychological.
- Early pain relief reduces anxiety
- Faster independence improves confidence
- Quicker return to work reduces financial stress
Patients who recover faster often show better long-term satisfaction and adherence to lifestyle advice.
Decision-Making: How Surgeons Choose the Right MISS Technique
Not all minimally invasive techniques are the same. Selection depends on:
- Exact pathology (disc, bone, ligament)
- Spinal level (cervical, thoracic, lumbar)
- Stability and alignment
- Patient occupation and activity demands
This individualized planning ensures maximum benefit with minimal risk.
Minimally Invasive Spine Surgery in Cervical Spine Disorders
MISS is not limited to the lower back.
- Cervical disc prolapse
- Cervical radiculopathy
- Selected cases of cervical myelopathy
Keyhole anterior or posterior approaches can decompress nerves while preserving neck mobility.
Role of Rehabilitation After MISS
Surgery corrects anatomy; rehabilitation restores function.
Phase 1: Early Mobilization
- Walking from day one
- Breathing and circulation exercises
Phase 2: Functional Strengthening
- Core muscle activation
- Hip and pelvic stability exercises
Phase 3: Return-to-Work Conditioning
- Job-specific movements
- Ergonomic retraining
This structured approach minimizes recurrence.
Preventing Recurrence After Spine Surgery
MISS significantly reduces recurrence risk, but patient participation is vital.
- Avoid smoking and tobacco
- Maintain optimal body weight
- Practice correct lifting techniques
- Continue prescribed exercises
Long-term spine health is a shared responsibility.
Cost-Effectiveness Over the Long Term
While minimally invasive surgery may appear costlier initially, overall economics favor MISS.
- Shorter hospital stay
- Earlier return to work
- Lower complication and reoperation rates
For working adults and families, this translates into substantial indirect savings.
Missed Opportunities: Risks of Delaying Surgery
Ignoring surgical indications can worsen outcomes.
- Permanent nerve damage
- Muscle weakness or foot drop
- Reduced surgical success later
Timely intervention often converts a simple MISS into a successful long-term solution.
Frequently Asked Concerns Addressed
“Will implants limit my movement?”
No. When indicated, implants stabilize only the affected segment while preserving overall spine mobility.
“Is endoscopic surgery suitable for everyone?”
No. Careful selection ensures safety and effectiveness.
“Can surgery be repeated if needed?”
Yes. MISS preserves anatomy, making future interventions easier if required.
Community Awareness & Patient Education
Education reduces fear and misinformation.
- Understanding that surgery is not always the first step
- Knowing that modern surgery is safer than before
- Recognizing red flags that need timely care
Well-informed patients make better decisions.
Global Standards, Local Expertise
Minimally invasive spine surgery practiced at high-volume centers in India, like Dr. Rao’s hospital, now matches international standards.
- Evidence-based protocols
- Continuous skill upgradation
- Outcomes comparable to global centers
This allows patients to receive world-class care close to home.
The Road Ahead for Spine Care in Andhra Pradesh
The future of spine care is shifting toward:
- Earlier diagnosis
- Motion-preserving surgeries
- Personalized rehabilitation programs
Minimally invasive techniques will remain central to this evolution.
Empowering Patients to Choose Wisely
The most successful outcomes occur when patients:
- Seek timely expert opinions
- Understand all available options
- Act before irreversible nerve damage
Informed choice leads to confident recovery.
Closing Perspective
Minimally invasive spine surgery is not just about smaller cuts—it is about smarter surgery. By combining precision, technology, and experience, it offers relief with dignity, speed, and safety.
For patients suffering from persistent back pain, sciatica, or spinal nerve compression, modern spine care provides hope without prolonged disability.
The right time, the right technique, and the right team can restore movement—and life itself.
Call to Action: If chronic back pain or sciatica is limiting your life, expert help is available.
For consultation with the best spine surgeon in Guntur and advanced minimally invasive spine surgery in Andhra Pradesh, visit Dr. Rao’s Hospital.
📞 090100 56444
📧 info@drraoshospitals.com
📍 Contact Dr. Rao’s Hospital
Facebook | Instagram | YouTube | LinkedIn | X (Twitter) | Google Maps
Inside the Operating Room: How MISS Is Actually Performed
Many patients imagine spine surgery as complex and intimidating. Understanding the actual steps of minimally invasive spine surgery often reduces fear and builds trust.
Step 1: Precise Localization
Using real-time imaging, the exact spinal level and pathology are identified before any incision is made. This prevents wrong-level surgery and unnecessary exposure.
Step 2: Small, Targeted Incision
An incision usually measuring 1–2 cm is made. Tubular retractors or endoscopic ports gently separate muscles instead of cutting them.
Step 3: Magnified Visualization
High-definition microscopes or endoscopes provide clear, magnified views of nerves, discs, and ligaments, allowing millimeter-level precision.
Step 4: Problem-Specific Correction
The surgeon removes only the offending disc fragment, bone spur, or thickened ligament—nothing more.
Step 5: Closure With Minimal Trauma
Because tissue damage is minimal, closure is quick and cosmetic, often with absorbable sutures.
Anesthesia in Minimally Invasive Spine Surgery
Advances in anesthesia play a key role in faster recovery.
- Shorter anesthesia duration
- Better pain control protocols
- Early awakening and mobilization
In selected cases, certain endoscopic spine surgeries can even be performed under regional anesthesia, reducing systemic stress.
Blood Loss, Transfusion & Safety Profile
One of the most reassuring aspects of MISS is minimal blood loss.
- Most procedures involve negligible blood loss
- Blood transfusion is rarely required
- Lower postoperative anemia risk
This makes MISS safer for elderly patients and those with medical comorbidities.
Infection Prevention & Wound Healing
Smaller incisions significantly reduce infection risk.
- Minimal tissue exposure
- Shorter operative time
- Faster wound healing
Patients often report excellent cosmetic outcomes with barely visible scars.
Minimally Invasive Spine Surgery for Recurrent Disc Herniation
Recurrent disc prolapse is a challenging condition. MISS offers clear advantages.
- Preserves previously operated tissues
- Reduces scar-related complications
- Allows focused re-decompression
This approach minimizes the need for larger revision surgeries.
MISS in Trauma & Selected Emergency Situations
While open surgery is still required in unstable trauma, MISS has a role in selected cases.
- Stable fractures with nerve compression
- Minimally displaced vertebral injuries
- Early stabilization with percutaneous techniques
These methods reduce hospital stay and speed up rehabilitation.
Understanding Pain After MISS: What Is Normal?
Some discomfort is expected after any surgery, but the pattern matters.
- Mild incision-site soreness for a few days
- Rapid reduction in leg or arm pain
- Minimal need for strong painkillers
Persistent or worsening pain is uncommon and should prompt evaluation.
Nerve Recovery: Why Patience Matters
Nerves heal more slowly than skin or muscle.
- Tingling or numbness may take weeks to months to resolve
- Strength improves gradually with rehabilitation
- Early surgery improves nerve recovery potential
This gradual improvement is normal and expected.
Role of Nutrition in Post-Surgery Recovery
Nutrition significantly influences healing.
- Adequate protein supports tissue repair
- Vitamin D and calcium aid bone health
- Hydration reduces muscle stiffness
Patients are counseled on simple dietary modifications to support recovery.
Driving, Travel & Daily Activities After MISS
Returning to normal routines is faster with MISS.
- Driving: Usually after 1–2 weeks (once pain-free)
- Short travel: Within days
- Long journeys: After medical clearance
Proper posture and breaks during travel are emphasized.
Sexual Activity & Intimacy After Spine Surgery
This topic is rarely discussed but important.
- Usually safe after pain subsides
- Avoid positions causing strain initially
- Gradual return based on comfort
Open communication with the care team helps address concerns.
MISS vs Alternative “Non-Surgical” Claims
Patients often encounter claims of permanent cures without surgery.
- Structural nerve compression cannot be reversed by medication alone
- Delaying necessary surgery may worsen outcomes
- Evidence-based care ensures lasting relief
MISS bridges the gap between conservative care and major surgery.
Ethical Decision-Making in Spine Surgery
Responsible spine care prioritizes patient benefit over procedures.
- Surgery recommended only when clearly indicated
- Conservative options discussed transparently
- Shared decision-making with patients and families
This ethical approach builds long-term trust.
Follow-Up Schedule After Minimally Invasive Spine Surgery
Structured follow-up ensures sustained success.
- Early wound check (7–10 days)
- Functional review at 4–6 weeks
- Long-term assessment at 3–6 months
Follow-ups focus on function, not just imaging.
Imaging After Surgery: When Is It Needed?
Routine scans are not always required.
- Imaging reserved for new symptoms
- Clinical recovery is the primary measure
- Avoids unnecessary radiation and cost
This patient-centered approach prevents over-investigation.
Comparing Outcomes: What Patients Value Most
Studies show patients prioritize:
- Pain relief
- Ability to return to work
- Long-term durability
MISS consistently scores high on all three parameters.
Role of Family Support in Recovery
Recovery improves with a supportive environment.
- Assistance during first few days
- Encouragement for walking and exercises
- Emotional reassurance
Educated families reduce anxiety and promote adherence.
Minimally Invasive Spine Surgery: A Paradigm Shift
The shift from large incisions to keyhole techniques represents a paradigm change in spine care.
- From prolonged bed rest to early mobility
- From fear of surgery to confidence in outcomes
- From disability to rapid reintegration into life
Final Thoughts for Patients Considering MISS
Choosing spine surgery is a major decision. Understanding modern minimally invasive options empowers patients to choose relief without unnecessary suffering.
With the right indication, experienced surgeon, and structured rehabilitation, minimally invasive spine surgery offers not just pain relief—but a return to normalcy.
Modern spine care is about precision, compassion, and restoring life—not just fixing the spine.
Quality Metrics That Define Successful Minimally Invasive Spine Surgery
Beyond pain relief, high-quality minimally invasive spine surgery (MISS) is measured using objective and patient-centered outcomes.
- Functional improvement: Ability to walk, sit, and work without limitation
- Neurological recovery: Improvement in strength, sensation, and reflexes
- Low complication rates: Infection, CSF leak, or reoperation
- Patient-reported outcomes: Satisfaction, confidence, and quality of life
Tracking these metrics ensures continuous improvement and accountability in spine care.
Importance of a Dedicated Spine Team
MISS outcomes depend not only on the surgeon but also on a coordinated multidisciplinary team.
- Spine-trained anesthesiologists
- Intraoperative neuromonitoring specialists
- Dedicated spine nursing staff
- Physiotherapists trained in post-spine surgery rehabilitation
This team-based approach reduces variability and enhances safety.
Training & Skill Development in Minimally Invasive Spine Surgery
MISS requires specialized training beyond conventional spine surgery.
- Cadaveric dissection workshops
- Endoscopic and microscopic simulation
- Mentorship under high-volume MISS surgeons
- Continuous skill upgradation with evolving technology
Surgeons trained in these techniques deliver consistently better outcomes.
Why High-Volume Centers Matter
Evidence shows that high-volume spine centers achieve:
- Lower complication rates
- Shorter operative times
- Better functional outcomes
Regular exposure to complex cases improves decision-making and technical precision.
Standardized Protocols vs Individualized Care
Modern spine care balances protocols with personalization.
- Standardized safety checklists
- Individualized surgical planning
- Customized rehabilitation pathways
This hybrid model ensures safety without sacrificing patient-specific needs.
Data-Driven Spine Care: Using Outcomes to Improve Practice
Outcome tracking is central to excellence.
- Pre- and post-operative functional scores
- Complication audits
- Long-term follow-up data
Analyzing these data points helps refine techniques and improve future care.
Role of Patient Education in Surgical Success
Informed patients recover better.
- Clear understanding of diagnosis
- Realistic expectations from surgery
- Active participation in rehabilitation
Education transforms patients from passive recipients into partners in care.
Prehabilitation: Preparing the Body Before Surgery
Prehabilitation improves surgical readiness.
- Core strengthening exercises
- Optimization of nutrition
- Control of blood sugar and blood pressure
Patients who undergo prehabilitation often experience smoother recovery.
Missed Red Flags: When MISS Should Not Be Delayed
Certain symptoms demand urgent surgical attention.
- Progressive weakness
- Loss of bladder or bowel control
- Severe unrelenting nerve pain
Early intervention prevents permanent neurological damage.
Addressing Fear & Anxiety Around Spine Surgery
Fear is natural but often fueled by outdated perceptions.
- Modern MISS is far less traumatic
- Most patients walk the same or next day
- Recovery timelines are predictable
Open discussion and counseling help patients approach surgery with confidence.
Ethics of Indication: Knowing When Not to Operate
Ethical spine care includes saying no to unnecessary surgery.
- Back pain without nerve compression
- Non-structural pain syndromes
- Conditions responding well to conservative care
Trust is built when surgery is recommended only when clearly beneficial.
Long-Term Surveillance After Minimally Invasive Spine Surgery
Spine health is lifelong.
- Periodic functional assessment
- Monitoring adjacent spinal segments
- Reinforcement of ergonomic habits
This proactive approach reduces recurrence and degeneration.
Return to Sports & Fitness After MISS
Many patients wish to resume active lifestyles.
- Walking and swimming: Early
- Yoga and cycling: Gradual reintroduction
- High-impact sports: After clearance
Guided progression prevents injury and builds confidence.
Women’s Health & Spine Surgery
Women may experience spine issues related to:
- Pregnancy-related biomechanical changes
- Osteoporosis
- Postural stress
MISS offers safer options with faster recovery and minimal disruption.
Occupational Spine Care: Desk Workers vs Manual Laborers
Recovery plans are tailored to occupational demands.
- Desk workers: Focus on posture and ergonomics
- Drivers: Emphasis on core strength and breaks
- Manual laborers: Gradual load reintroduction
This customization ensures sustainable return to work.
Global Evidence Supporting Minimally Invasive Spine Surgery
International studies consistently demonstrate:
- Equivalent or superior outcomes compared to open surgery
- Lower complication rates
- Higher patient satisfaction
This evidence underpins the global shift toward MISS.
Building Trust Through Transparency
Transparency strengthens patient trust.
- Clear explanation of risks and benefits
- Open discussion of alternatives
- Honest communication about recovery timelines
Trust enhances adherence and outcomes.
From Pain to Performance: Redefining Success
Success is not merely absence of pain—it is restored performance.
- Ability to work productively
- Participation in family and social life
- Confidence in movement
MISS aims to restore function, not just anatomy.
The Patient’s Role in Long-Term Spine Health
Surgery is a milestone, not the finish line.
- Adherence to exercise programs
- Mindful posture and movement
- Regular health check-ups
Active participation ensures lasting benefits.
Looking Forward: The Evolution Continues
The field of spine surgery continues to evolve.
- Smaller instruments
- Enhanced visualization
- More motion-preserving solutions
Minimally invasive spine surgery will remain at the heart of this progress.
Enduring Message for Patients
Back pain and spine disorders need not dictate your life. With timely evaluation, ethical guidance, and modern minimally invasive solutions, recovery is achievable.
Choose knowledge over fear, precision over trauma, and recovery over resignation.
Call to Action: If chronic back pain or sciatica is limiting your life, expert help is available.
For consultation with the best spine surgeon in Guntur and advanced minimally invasive spine surgery in Andhra Pradesh, visit Dr. Rao’s Hospital.
📞 090100 56444
📧 info@drraoshospitals.com
📍 Contact Dr. Rao’s Hospital
Facebook | Instagram | YouTube | LinkedIn | X (Twitter) | Google Maps