How Technology Is Redefining Patient Safety in Brain & Spine Surgery
Patient safety has always been the cornerstone of neurosurgery. Brain and spine surgery deal with the most delicate and functionally critical structures of the human body. Today, technology is redefining patient safety in brain and spine surgery by dramatically reducing risks, improving precision, and enhancing recovery. From neuronavigation and intraoperative neuromonitoring to AI-assisted planning and smart operating rooms, modern neurosurgery has entered a new era of safety-driven care.
This transformation is especially visible in advanced neurosurgery centers in India, where cutting-edge technology is being integrated into routine clinical practice, making complex brain and spine surgery safer than ever before.
Why Patient Safety Is Critical in Brain & Spine Surgery
The brain and spinal cord control movement, sensation, speech, vision, memory, and every vital function. Even minimal injury can result in permanent neurological deficits. Historically, neurosurgery carried significant risks of paralysis, speech loss, sensory deficits, infection, and prolonged recovery.
Modern neurosurgery patient safety focuses on:
- Preventing neurological injury
- Reducing blood loss and infection risk
- Improving surgical accuracy
- Enhancing recovery and quality of life
Technology is now the primary enabler of these safety goals.
How Technology Improves Patient Safety in Neurosurgery
1. Neuronavigation & Image-Guided Neurosurgery
Neuronavigation acts as a GPS system for the brain and spine. Using preoperative MRI and CT scans, surgeons can navigate complex anatomy in real time. Navigation-guided brain and spine surgery significantly improves accuracy and reduces damage to surrounding healthy tissue.
Benefits for patient safety include:
- Precise localization of tumors and spinal pathology
- Safer placement of pedicle screws and implants
- Reduced risk of nerve and spinal cord injury
- Lower revision surgery rates
Studies indexed on PubMed show navigation-guided surgery improves pedicle screw accuracy
to over 95% compared to freehand techniques.
[Source: PubMed]
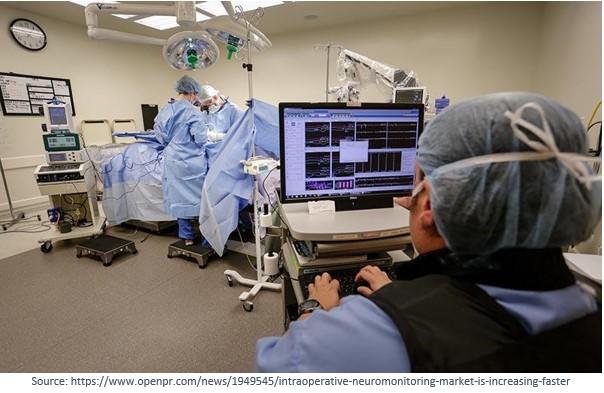
2. Intraoperative Neuromonitoring (IONM)
Intraoperative neuromonitoring (IONM) has become a cornerstone of patient safety in brain and spine surgery. IONM continuously monitors neural pathways during surgery, alerting the surgical team to potential injury in real time.
Common modalities include:
- Somatosensory Evoked Potentials (SSEP)
- Motor Evoked Potentials (MEP)
- Electromyography (EMG)
- Cranial nerve monitoring
IONM plays a critical role in:
- Preventing paralysis during spine surgery
- Protecting speech and motor function during brain surgery
- Reducing permanent neurological complications
IONM is now considered a standard of care for high-risk neurosurgical procedures worldwide.
3. Minimally Invasive & Endoscopic Techniques
Minimally invasive brain and spine surgery has dramatically improved patient safety. Smaller incisions, minimal tissue disruption, and targeted approaches reduce surgical trauma.
Advantages include:
- Reduced blood loss
- Lower infection risk
- Less postoperative pain
- Faster mobilization and recovery
Endoscopic brain surgery and endoscopic spine surgery allow surgeons to operate through natural corridors or keyhole approaches, preserving normal anatomy and function.
According to Mayo Clinic data, minimally invasive techniques are associated with shorter hospital stays and fewer complications. [Source: Mayo Clinic]
4. AI-Assisted & Computer-Guided Neurosurgery
Artificial intelligence is emerging as a powerful tool in neurosurgery. AI-assisted neurosurgery enhances patient safety by improving preoperative planning, risk stratification, and intraoperative decision-making.
AI applications include:
- Automated image analysis
- Tumor margin prediction
- Trajectory planning for complex surgeries
- Outcome prediction models
AI-driven insights help surgeons anticipate complications and tailor surgical strategies for each patient, further reducing risk.
5. Robotic & Computer-Assisted Spine Surgery
Robotic and computer-assisted spine surgery improves implant placement accuracy and consistency. These systems enhance stability and reduce human error, especially in complex deformity correction and revision surgeries.
Safety benefits include:
- Improved screw placement accuracy
- Reduced radiation exposure
- Lower revision surgery rates
6. Advanced Neuro ICU & Smart Operating Rooms
Patient safety extends beyond the operating table. Advanced Neuro ICU technology enables continuous monitoring of intracranial pressure, cerebral oxygenation, and vital neurological parameters.
Smart operating rooms integrate:
- Real-time imaging
- Digital data capture
- Team communication systems
These technologies support faster intervention in emergencies and improve postoperative outcomes.
Technology-Driven Outcomes in Brain & Spine Surgery
Technology has led to measurable improvements in neurosurgical outcomes:
- Lower neurological complication rates
- Reduced blood loss and transfusion needs
- Shorter hospital stays
- Faster functional recovery
WHO emphasizes that technology-driven safety systems are essential to reducing surgical complications globally. [Source: WHO]
Technology-Driven Patient Safety in India
India has rapidly emerged as a leader in advanced neurosurgery technology. Centers across the country now offer navigation-guided surgery, IONM, endoscopic approaches, and AI-assisted planning.
This technological advancement has made high-quality, safe neurosurgical care accessible and cost-effective, benefiting both domestic and international patients.
Technology & Patient Safety at Dr. Rao’s Hospital, Guntur
At Dr. Rao’s Hospital, technology-driven patient safety is central to every brain and spine surgery. Under the leadership of Dr. Mohana Rao Patibandla, the hospital integrates:
- Neuronavigation-guided brain and spine surgery
- Comprehensive intraoperative neuromonitoring
- Minimally invasive and endoscopic techniques
- Advanced Neuro ICU care
This approach ensures safer surgeries, better outcomes, and faster recovery for patients in Guntur and across Andhra Pradesh.
Frequently Asked Questions (FAQ)
How does technology improve patient safety in neurosurgery?
Technology improves neurosurgery safety by increasing precision, enabling real-time monitoring, reducing complications, and supporting faster recovery.
Is navigation-guided surgery safer than traditional methods?
Yes. Navigation-guided surgery significantly improves accuracy and reduces the risk of nerve and spinal cord injury.
Why choose Dr. Rao’s Hospital for technology-driven neurosurgery?
At Dr. Rao’s Hospital, patients receive advanced, compassionate care using state-of-the-art technology under the expertise of Dr. Mohana Rao Patibandla.
Consult a Technology-Driven Neurosurgery Expert
If you are searching for the best neurosurgeon in Guntur or the safest brain and spine surgery near you, visit Dr. Rao’s Hospital.
📞 Call: 090100 56444
📧 Email: info@drraoshospitals.com
📍 Location: Guntur, Andhra Pradesh
Follow Dr. Rao’s Hospital
- YouTube
Advanced Neurosurgery in Guntur
Comprehensive Neurology Care in Guntur
Advanced Spine Surgery in Guntur
Minimally Invasive Brain and Spine Surgery
Pediatric Neurosurgery in Guntur
Advanced Epilepsy Surgery in Guntur
Technology. Precision. Safety. The Future of Neurosurgery.
The Bigger Impact: Safer Surgery, Better Lives
The true success of technology in neurosurgery is measured not only in surgical precision, but in preserved neurological function, faster recovery, and improved quality of life. When advanced tools are used responsibly and expertly, patients experience fewer complications,
shorter hospital stays, and a smoother return to daily activities.
Technology also empowers informed decision-making. Data-driven neurosurgery, supported by real-time monitoring and evidence-based protocols, allows surgeons to adapt instantly to changing intraoperative conditions, placing patient safety above all else.
As neurosurgical technology continues to evolve through 2025 and 2026, the focus is shifting from merely “successful surgery” to predictable safety, functional preservation, and long-term outcomes.
Technology Is Only as Powerful as the Hands That Use It
While advanced neurosurgical technology is transformative, its true value depends on the surgeon’s experience, judgment, and ethical practice. High-end tools must be combined with deep anatomical knowledge, multidisciplinary teamwork, and patient-centered care.
Centers that invest not only in equipment but also in training, protocols, and outcome monitoring are redefining what safe brain and spine surgery means today.
Choose a Technology-Driven, Safety-First Neurosurgery Center
If you or your loved one requires brain or spine surgery, choosing a hospital that prioritizes technology-driven patient safety can make a critical difference in outcomes.
At Dr. Rao’s Hospital in Guntur, advanced neurosurgical technology is integrated into every stage of care—from diagnosis and surgical planning to intraoperative monitoring and postoperative recovery.
Under the leadership of Dr. Mohana Rao Patibandla, patients benefit from navigation-guided surgery, intraoperative neuromonitoring, minimally invasive techniques, and comprehensive Neuro ICU support, ensuring the highest standards of safety in brain and spine surgery.
Book a Consultation
If you are searching for the best neurosurgeon in Guntur, or expert care for complex brain and spine conditions using the safest modern neurosurgical techniques, we are here to help.
👉 Visit: https://drraoshospitals.com
📞 Call: 090100 56444
📧 Email: info@drraoshospitals.com
📍 Location: Guntur, Andhra Pradesh
Stay Connected with Dr. Rao’s Hospital
Follow us for updates on neurosurgical innovations, patient education, and technology-driven outcomes:
- 📘 Facebook: facebook.com/Dr.Raoshospital.Neurosurgeon
- 📸 Instagram: @dr_mohana_rao
- 📺 YouTube: Dr. Mohana Rao Patibandla
- 💼 LinkedIn: linkedin.com/in/drpatibandla
- 🐦 X (Twitter): @MohanaRaoPatib
Advanced Technology. Precision Surgery. Uncompromising Patient Safety.
People Also Ask: Patient Safety in Brain & Spine Surgery
How does technology improve patient safety in brain and spine surgery?
Technology improves patient safety in brain and spine surgery by enhancing precision, enabling real-time neural monitoring, reducing blood loss, preventing nerve injury, and supporting faster recovery.
Is navigation-guided brain and spine surgery safer?
Yes. Navigation-guided surgery is significantly safer than conventional techniques because it allows accurate localization of critical structures, improves implant placement, and reduces surgical errors.
What is intraoperative neuromonitoring and why is it important?
Intraoperative neuromonitoring (IONM) continuously tracks brain, spinal cord, and nerve function during surgery, helping prevent permanent neurological damage.
Does minimally invasive neurosurgery reduce complications?
Minimally invasive brain and spine surgery reduces complications by minimizing tissue damage,
lowering infection risk, decreasing pain, and enabling faster mobilization.
Is advanced neurosurgical technology available in India?
Yes. Leading neurosurgery centers in India now offer neuronavigation, intraoperative neuromonitoring, endoscopic techniques, and AI-assisted planning at global standards.
How do patients benefit from technology-driven neurosurgery?
Patients benefit through safer surgery, better preservation of neurological function, shorter hospital stays, faster recovery, and improved long-term outcomes.
Summary: Technology Is Transforming Neurosurgical Safety
Technology is redefining patient safety in brain and spine surgery by shifting the focus
from risk mitigation to precision-driven, outcome-based care. With the integration of neuronavigation, intraoperative neuromonitoring, minimally invasive techniques, AI-assisted planning, and advanced Neuro ICU support, modern neurosurgery is safer than ever before.
When advanced technology is combined with surgical expertise and ethical practice, patients experience fewer complications, faster recovery, and better preservation of neurological function.
Consult a Technology-Driven Neurosurgery Expert
If you are searching for the best neurosurgeon in Guntur
or a hospital that prioritizes patient safety in brain and spine surgery,
expert care is within reach.
At Dr. Rao’s Hospital, technology-driven neurosurgery is delivered under the leadership of
Dr. Mohana Rao Patibandla, with a strong focus on safety, precision, and compassionate care.
👉 Visit: https://drraoshospitals.com
📞 Call: 090100 56444
📧 Email: info@drraoshospitals.com
📍 Location: Guntur, Andhra Pradesh
Follow Dr. Rao’s Hospital
Stay informed about advances in neurosurgery, patient safety innovations,
and expert insights:
- 📘 Facebook: facebook.com/Dr.Raoshospital.Neurosurgeon
- 📸 Instagram: @dr_mohana_rao
- 📺 YouTube: Dr. Mohana Rao Patibandla
- 💼 LinkedIn: linkedin.com/in/drpatibandla
- 🐦 X (Twitter): @MohanaRaoPatib
Precision Technology. Expert Hands. Safer Brain & Spine Surgery.