When Should the Spine Surgery Be Considered?
Most people experience at least one major bout of back pain at some point in their life. While surgery may appear to be an excellent option to address chronic back pain, it is not always necessary. For many people, spinal surgery is ineffective, leading to persistent or even worse discomfort. However, there are a few instances when surgery is the best option. Dr. Raos Hospital is the best spine surgery hospital in Guntur and Andhra Pradesh and offers the best minimally invasive neurosurgery by the best Neurosurgeon in India, DR RAO. According to mid-day
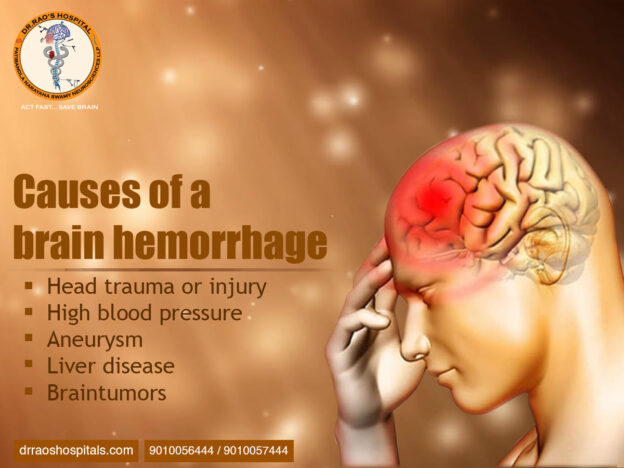
Infection, trauma, neurological dysfunction, tumors, or significant structural abnormalities such as scoliosis are reasons for spine surgery. The final reason for surgery is pain that has not responded to more conservative treatments and imaging evidence that suggests a surgically correctable anomaly that, if operated on, could provide pain relief.
This article will review a few of these scenarios to help you determine what kind of treatment is best for you.
Let’s know,
When Is Spine Surgery Needed?
Interventional pain treatment offers many non-surgical options for treating a patient’s pain. The most common treatments are physical therapy, medicines, anti-inflammatories, and lifestyle changes. Exploring more conservative non-surgical methods before considering spine surgery is always a good idea.
At Dr. Rao’s Hospital, one of the best neurology hospitals in Guntur, Andhra Pradesh, proficient spine surgeons can often aid when these therapeutic choices fail to offer relief. Some available treatments include epidural steroid injections, nerve blocks, nerve ablations, regenerative medicine (i.e., PRP and stem cell treatments), and spinal cord stimulation (SCS).
Our surgeons may recommend surgery if non-surgical treatments fail to relieve the back discomfort. Our well-qualified and seasoned surgeons aim to provide the best spine surgery treatment in Andhra Pradesh. Patients with ruptured discs, spondylolisthesis, spinal fractures, and degenerative disc disease are good candidates for surgery.
Besides, it is worth noting that, even in these cases, surgery should only be considered if the particular source of the discomfort has been identified, for example, a herniated disc, scoliosis, or spinal stenosis. You may be a candidate for spinal surgery if the source of your pain has been identified and non-surgical treatments have failed.
How Serious Is Spine Surgery?
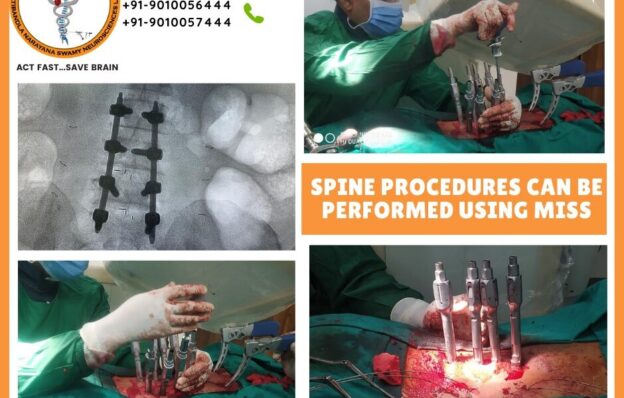
Your type of surgery determines the severity of your back surgery. Traditional open surgery or minimally invasive spine surgery (MISS) are also options for spinal surgery.
MISS avoids open manipulation of the muscles and tissues around the spine and does not require extensive incisions. As a result, patients frequently recover faster and with less discomfort.
Due to its proximity to the nerve system, back surgery carries a higher risk than other forms of surgery. Paralysis and infection are the most severe risks. While the risks of open spinal procedures and MISS are roughly the same, certain studies suggest that MISS has a lower risk of infection than traditional back surgery.
In the case of spinal fusions, other potential consequences include bleeding, prolonged discomfort at the graft site, reoccurring symptoms, nerve injury, blood clots, and pseudarthrosis.
MISS techniques enable patients to stay in the hospital less often, with most leaving home the same day or within 1 to 2 days. On the other hand, standard surgery usually requires 3 to 5 days in the hospital. The recovery period can be lengthy and painful even if the surgery is successful. Pain management and physical therapy will be required for the majority of individuals.
What Is The Success Rate Of Spine Surgery?
The success of spine surgery is determined by the surgical procedures used. For example, the success rate of lumbar spinal fusion, as judged by pain reduction, is frequently less than 80%. Furthermore, despite immediate pain reduction success, many lumbar spine procedures fail within 3 to 5 years. This is due to changes in the biomechanical structure of the spine due to the surgery, which causes issues in adjacent spinal levels.
Because so many spine procedures fail, there is a medical term for this: failed back surgery syndrome. This low success rate can be attributed to several factors. The most important is that the site operated on was not the source of the patient’s suffering. This is why, before undergoing spine surgery, it’s critical to pinpoint the particular source of pain.
In conclusion, surgery is not “necessary” for most patients with back pain and sciatica. However, if you believe you are a candidate for surgery, you should seek a second opinion before proceeding. This will not only determine whether surgery is genuinely essential, but it will also ensure that you receive the best sort of surgery and the least invasive technique feasible.
Contact us today to schedule a complete physical exam, imaging review, and evaluation so our expert spine surgeons can identify the best appropriate treatment strategy for your persistent back pain and sciatica.
Dr. Rao’s Contact Information:
- Phone: 9010056444, 9010057444
- Email: info@drraoshospitals.com
- Address: Old Bank St, GV Thota, beside AK Biryani Point, Guntur, Andhra Pradesh 522001
- Website: Dr. Rao’s Hospital